Fractures of the process of the lower spine or upper thoracic spine are often referred to as clay-shoveler’s fractures.
Initially reported in 1940, these fractures were described among employees in Australia who dug drains in clay soil and also threw the clay overhead with shovels. The mud wouldn’t discharge from the spade, causing excess power to be transmitted into the supraspinous ligaments and leading to an avulsion fracture of one or more spinous processes.
The following frequently describes the mechanism of injury for clay shoveler’s fractures. The contraction of the paraspinal and trapezius muscles on the ligaments along with the attachment to the spinous processes make this a common injury during athletics with a flexed position of the shoulders and neck. The consequent fracture or apophyseal avulsion is painful and frequently requires a visit to the doctor, together with plain films, computed tomography (CT) scans, or magnetic resonance imaging (MRI) confirming the identification.
Often a period of rest will allow a return to activity, although treatment of these fractures hasn’t been clarified. We present a collection of adolescent athletes who underwent surgical interventions to treat the fracture of the spinous process, after rest and physical therapy with persistent symptoms.
Table of Contents
Surgical Intervention Study
Dr. Hedequist operated on 3 patients using a spinous process nonunion within the study time period. The patients’ average age was 14 years; the location of the spinous process fracture was the T1 vertebra in all patients. Two patients sustained the injury while playing hockey and one while wrestling. The average duration of symptoms before surgery was 10 months; all patients had seen physicians without a diagnosis before test in institution. All patients had a trial of physical therapy and all had been unable to return after trauma to pain.
Examination of patients showed pain directly over the fracture site and accentuated by forward flexion of the neck and neck. Evaluation of harm plain films revealed a fracture fragment in two patients (Figure 1). All 3 patients underwent CT and MRI scans confirming the identification. MRI confirmed areas of increased signal at the tip of the T1 spinous process, with inflammation in the supraspinous ligament directly at that area (Figure 2). The CT scans confirmed the presence of a bony fragment correlating with the suggestion of the T1 spinous process (Figure 3).
Figure 1
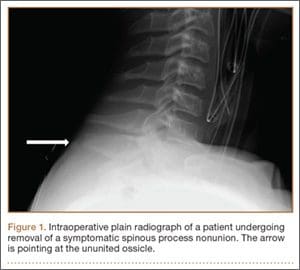
Figure 2
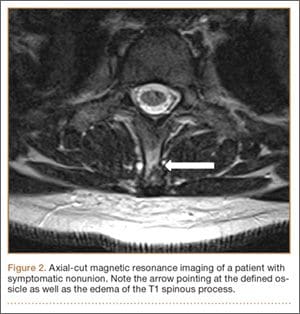
Figure 3
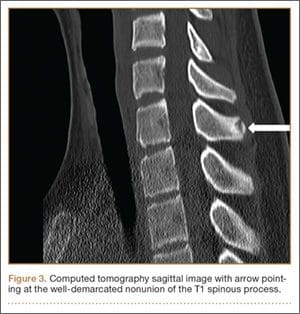
Surgery was performed under general endotracheal anesthesia using a midline incision over the affected region down to the spinous procedure. The supraspinous ligament was opened showing an identified and ununited ossicle, which has been removed without taking down the ligament. All 3 nonunions have been noted to be atrophic with no evidence of surrounding inflammatory tissue or bursa. The residual end of the spinous process was smoothed down with a rongeur. Standard closure was performed. There were no surgical complications.
All patients had complete relief of pain at followup; 1 individual returned to full sports activity at 6 months and the other 2 returned to full sports activity at 3 months. There was no loss of peripheral movement or trapezial strength at follow-up. All patients expressed satisfaction together with the decision.
Discussion
Clinical practice suggests that most patients with spinous process fractures will become pain-free; however, that is not universal. This series demonstrates that a tiny subset of patients with this trauma will continue to have significant symptoms despite a period of rest. In those patients who want a yield to sports, we recommend consideration of surgical excision after confirmation of nonunion with studies. The inherent risks of surgical treatment are minimal with this procedure, and the advantages include return for athletes, with the physical and psychosocial benefits to pain-free sports activity.
The scope of our information is limited to chiropractic and spinal injuries and conditions. To discuss options on the subject matter, please feel free to ask Dr. Jimenez or contact us at 915-850-0900 . 
By Dr. Alex Jimenez
Additional Topics: Automobile Accident Injuries
Whiplash, among other automobile accident injuries, are frequently reported by victims of an auto collision, regardless of the severity and grade of the accident. The sheer force of an impact can cause damage or injury to the cervical spine, as well as to the rest of the spine. Whiplash is generally the result of an abrupt, back-and-forth jolt of the head and neck in any direction. Fortunately, a variety of treatments are available to treat automobile accident injuries.
<
div class=”video-container”>
<
iframe src=”https://www.waxwinginteractive.com/manage/admin/playembed.php?vid=2&client=1350 scrolling=”no” border-width=”0″>

TRENDING TOPIC: EXTRA EXTRA: New PUSH 24/7Â®ï¸ Fitness Center
Post Disclaimer
Professional Scope of Practice *
The information herein on "Surgical Interventions for Cervical Spinous Process Fractures" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness, Personal Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those on this site and our family practice-based chiromed.com site, and focuses on restoring health naturally for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
Licenses and Board Certifications:
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card





 Again, We Welcome You.
Again, We Welcome You.
Comments are closed.