In the first part of this 2-part article, chiropractor, Dr. Alexander Jimenez looks at the surgery and rehab Alternatives for Femoro – Acetabular Impingement (FAI), a increasingly common musculoskeletal disorder that can affect young to middle aged athletes. In part two, Dr. Jimenez will describe in detail the postoperative rehabilitation interval required to have an athlete back to full competition
Table of Contents
Introduction
A potential cause of hip arthritis and degeneration was originally indicated by Stulberg et al (1975), even when they identified the ‘pistol grip deformity’ from the x-ray signs of abnormal head of femur (HOF) clearance from the acetabulum in patients with hip arthritis(1). This resulted in the idea that mechanical impingement could possibly be among those underlying causes of hip degeneration and hip joint pain.
Over the next few decades, with Improvements in radiology and hip joint surgery, and more complex clinical assessment skills, it was recognized that a number of atypical hip joint morphologies often existed that may contribute to hip joint pain in athletes.
In the late 1990’s, Mayer et al (1999)(two) Were the first to use the word ‘Femoro- acetabular impingement’ or ‘FAI’ to explain the morphology of the hip as being a causative factor in hip joint arthritis, and the notion of FAI was further initiated by Reinhold Ganz(3) and colleagues during the early 2000s.
An FAI is a real complication for an athlete, especially for young male athletes, because it cannot only cause hip joint pain and labral and cartilage damage, but it can also contribute to other athletic injuries like osteitis pubis and cerebral hernias due to the detrimental effect that too little hip joint rotation plays on thoracic strain injuries(4). The purpose of this rehabilitation Masterclass would be to explain the appropriate anatomy and biomechanics of the hip joint, explain the pathogenesis of both FAI and offer management ideas and also an in depth overview of the rehabilitation of the hip joint post-FAI operation.
Relevant Anatomy & Biomechanics
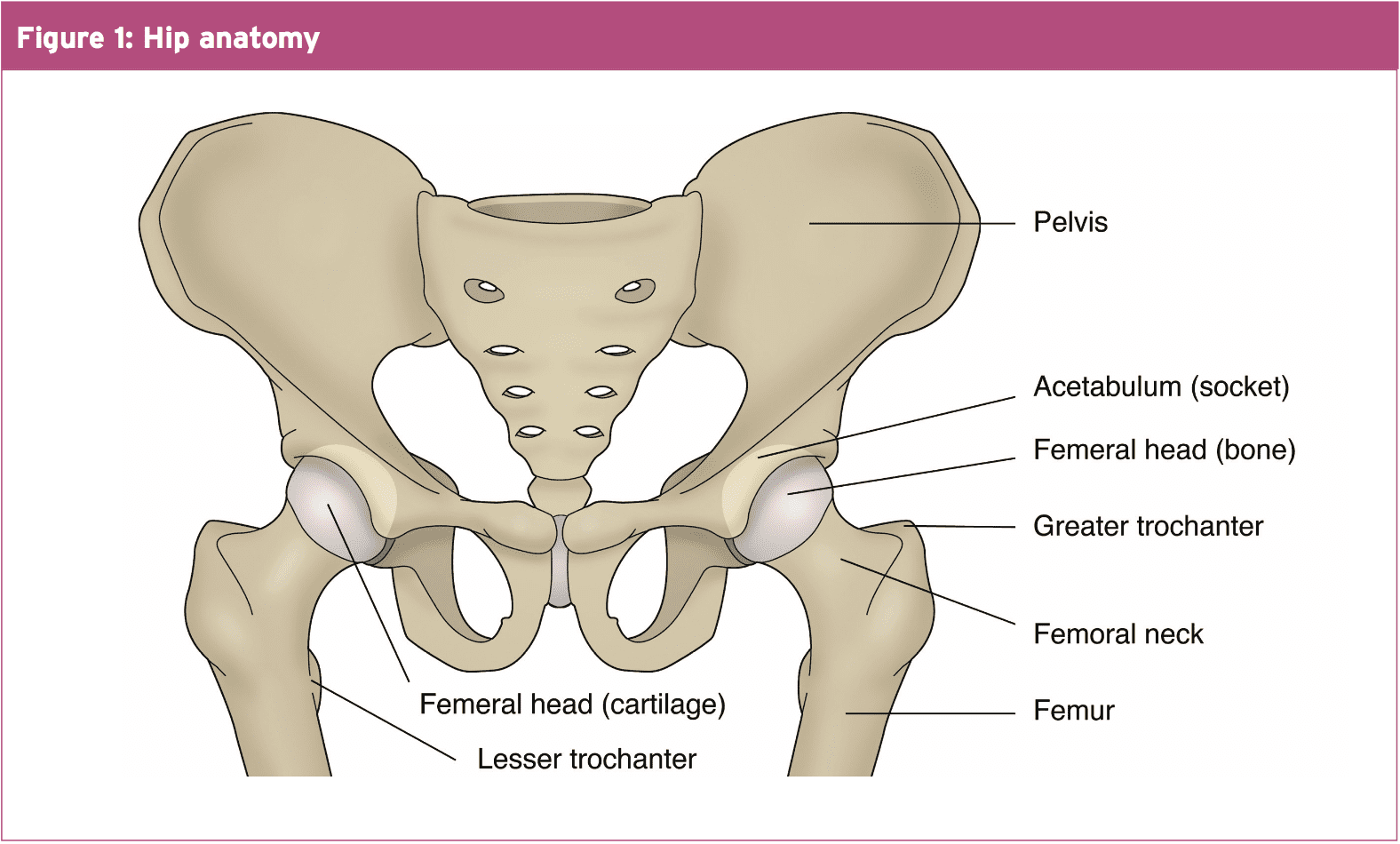 The hip joint is a ball and socket joint that has a wide range of movement into all planes of motion.
The hip joint is a ball and socket joint that has a wide range of movement into all planes of motion.
- The head is slightly more than half a sphere.
2. The femoral neck is cylindrical, narrowest in the midpoint and widest laterally, and attaches the head to the shaft.
- The acetabulum is cup shaped.
-
The labrum is triangular in cross section using its base attached to the acetabular rim.
Usually a space is maintained between the Femoral head neck junction and the acetabular rim, and this provides unhindered hip motion. The normal head cancel is 9 mm(6 feet).
Symptoms
Lead to impingement kind symptoms. A deviation from the standard alignment of the hip can cause a mechanical blockage between the acetabular rim and/ or head-neck of femur. This deviation away from the ordinary may be due to inherent geometry flaws from the patient’s hip joint complicated.
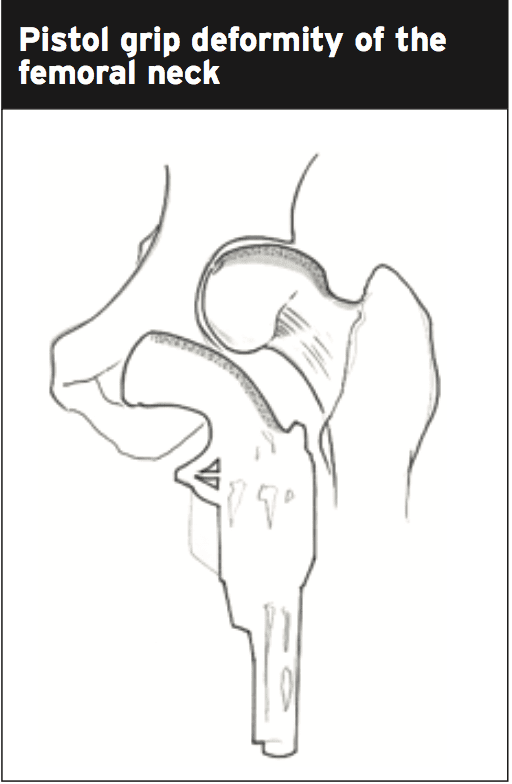
- Pistol grip deformity of the femoral neck.
-
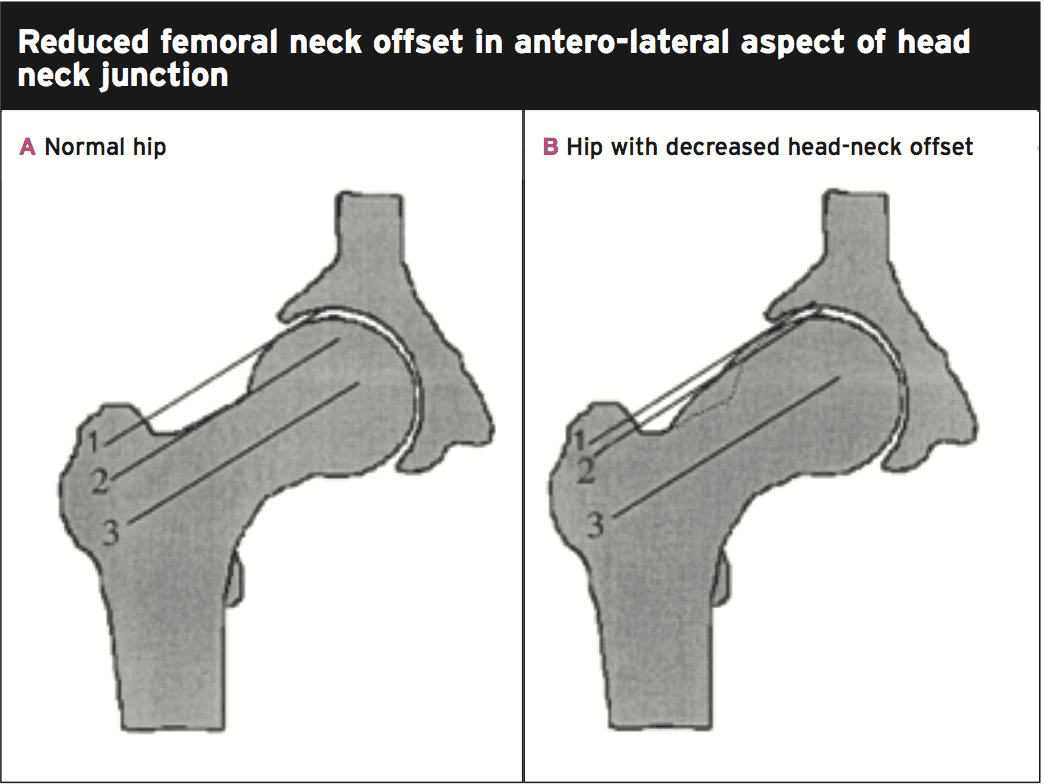
Reduced femoral neck offset in anterolateral aspect of head neck junction.
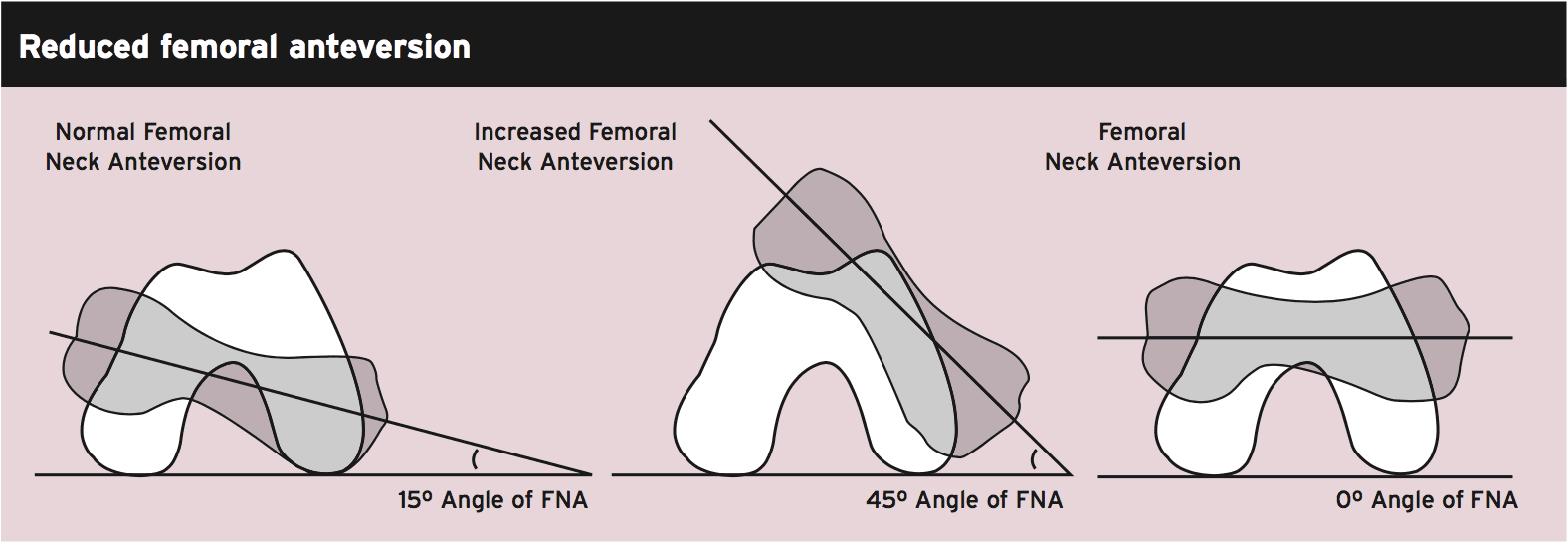
- Reduced femoral anteversion.
- Loss of spherecity from the femoral head.
-
Excessive coverage of acetabulum
-
Retroversion of acetabulum (causes over-coverage and restricts flexion of the femoral neck).
- Coxa profunda deformity floor of the acetabulum touches the ilio-ischial line) increases the depth of the acetabulum.
FAI As Injury
Although some examples of hip joint Impingement are caused by inherent hip joint abnormalities, FAI as an injury is an anatomical mal-alignment between the head and neck of femur and the acetabulum. This causes compression of the labrum and articular cartilage through hip flexion demonstrating as anterior hip pain and development to premature osteoarthritis of the hip. It is a state that seems to influence younger active men and women, particularly men. For instance, in a radiological analysis of 155 young active individuals 18-50 decades old with complaints of hip pain, it had been discovered that a staggering 87 percent of subjects had evidence of an FAI(7).
The natural development of an FAI to Since the labrum frays along the thoracic borders, this progresses into a more consequential tear of the labrum. The articular cartilage then delaminates away from the articular margin adjacent to the labral lesion. This subsequently contributes to unnatural shear forces throughout the joint, which over a long expression, induces more international labral and articular degeneration.
Furthermore, more recent research Suggests a strong link between FAI and other athletic groin pain syndromes, in particular athletic pubalgia. Economopoulos et al (2014) found that in 43 patients who underwent operation for athletic pubalgia, 86% of these had evidence of a FAI in a minumum of one hip, together with Cam lesions being the most prevalent (see below for Cam lesion)(9). This highlights the possible interaction between forces acting across the pelvis and hip joint. Hammoud et al (2014) supply an in-depth discussion on the way the FAI can potentially lead mechanical reimbursement routines, which can subsequently result in a plethora of sports injuries like osteitis pubis, sacroiliac joint problems, posterior hip impingement and proximal hamstring syndrome simply to name a few(10).
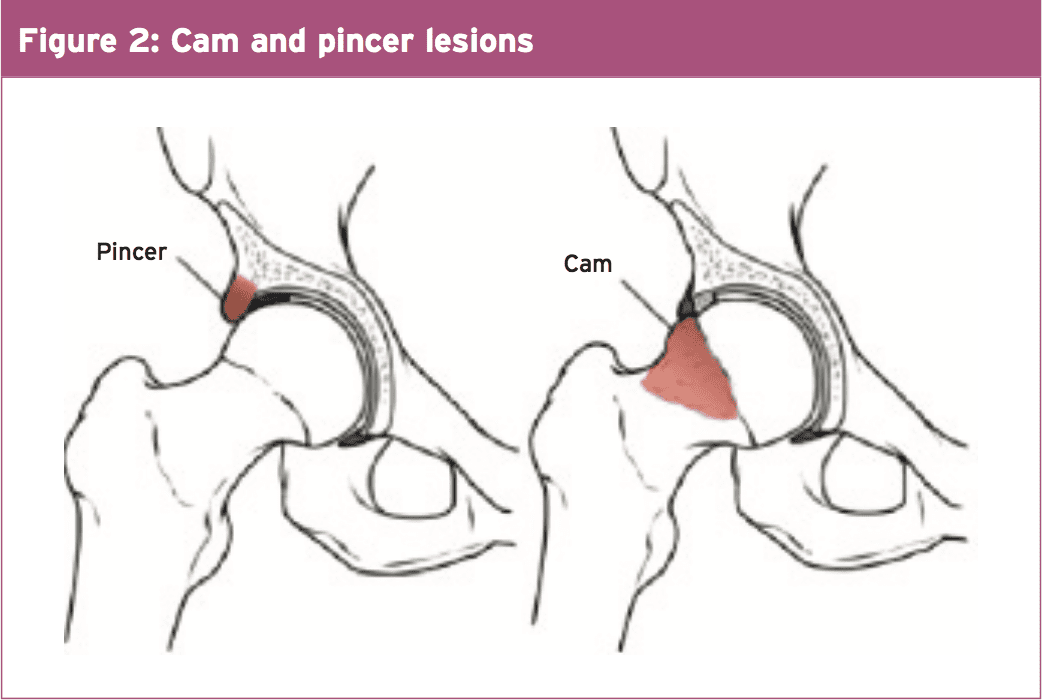
In the context of FAI, two primary Manifestations of FAI are described. These are ‘Cam’ and ‘Pincer’ lesions (see figure 2).
 Cam Lesions
Cam Lesions
The Cam lesion is attributed to an Asymmetric or non-spherical section of the femoral head or neck abutting from an acetabular rim. This abutment is the most evident in flexion and internal rotation where a shear force happens along the anterolateral edge of the acetabulum. This deformity reduces the mind neck counter, raises the femoral head radius of curvature and results in relative retroversion of the femoral head.
The smooth motion between the Femoral head and acetabulum is missing, which causes an outside-in abrasion of the acetabular cartilage with avulsion in the labrum and subchondral bone (delamination). This may result in separation of the cartilage in the antero superior part of the labrum(11). Labral injuries are more likely to affect the anterior region possibly due to its inadequate blood supply.
Cam lesions are typical in young Active guys with a ratio of around 25 percent in asymptomatic hips(13), and around 78 percent in thoracic hips(14). It’s more prevalent in males than in women at a ratio of 3:1(15). It is possible that a major factor in the development of a Cam lesion is a slipped capital femoral epiphysis where posterior displacement of this capitis leaves a prominence of the anterior neck, leading to severely limited internal rotation of the hip(16). Furthermore pistol grip deformities may result in more subtle forms of aspherical mind of femurs, and these have been correlated with early onset osteoarthritis in adults.

Pincer Lesions
Pincer lesions produce repeated contact between a normal femoral head neck and an over coated acetabular rim. This causes multiple cleavage planes in the labrum and subsequent labral degeneration, intrasubstance ganglion formation, ossification of the acetabular rim, and ultimately a portion of the acetabulum further compounding the pincer lesion.
Unlike in cam lesions, the chondral Harm associated with pincer lesions is much more circumferential in the anterior and supero-lateral acetabular rim, where force transmission is larger and as a ‘contre- coup’ lesion in the posterior capsular- labral junction as the ‘levering’ from the femoral head along the fulcrum generated by the anterior pincer lesion whilst the hip is bending(17,18).
Retroversion of the pelvis can also cause the acetabular rim to roll backward. It’s to be noted that spinal deformities like scoliosis or kyphosis can cause pelvic rotation and practical retroversion of the acetabulum that might work as a pincer lesion. There can also be an extra bit of bone along the lateral rim of the acetabulum known as an ‘os acetabulum'(19). Pincer lesions are more frequent in busy females(20).
 Mixed Lesions
Mixed Lesions
Rarely do cam and pincer lesions happen in isolation. Most type of FAI happens from mixed cam and pincer pathology at the But, Cobb et Al. (2010) argued against that after Analyzing the morphology of 60 acetabula Using CT scans(21). They reported that Acetabula with cam hips were shallower Than ordinary hips, which subsequently were Hence, they Concluded, that camera and pincer lesions Were different patho-anatomic entities With camera hips being shallow while the Pincer hips are deeper than normal hips.
Signs & Symptoms of FAI
FAI in the athlete may pose as insidious onset groin pain worsened by hip flexion and hip flexion with internal rotation type movements. It is more common in male athletes on account of the male inclination towards Cam impingements. Sports with a higher incidence of FAI are sports which involve a great deal of forced flexion with inner rotation including treading water polo, breaststroke kicking, football sports like football and AFL, rugby, field hockey, combat sports like wrestling and Brazilian Jujitsu and ice hockey.
The athlete themselves might aid the identification by providing information regarding childhood diseases that could result in abnormal head throat junctions. Conditions for example Perthes disease (3-12 year olds) or slipped capital femoral epiphysis (SCFE) (12-14 year olds) may alert the sports medicine practitioner an underlying FAI could be present.
The typical collection of symptoms and signs are;
- Insidious onset of symptoms at active young and middle aged adults.
-
Groin pain associated with action and no prior history of trauma.
-
Inability to perform tasks such as high hip flexion or extend sitting.
-
May hurt moving from squat or sit to standing.
-
Sharp stabbing pain with motions like aggressive turning or pivoting.
-
Painful clicking, locking or instability out of a labral tear leading to undiagnosed FAI.
-
Reduced range of motion especially flexion, adduction and internal rotation. Often athletes notice that they are less elastic as their team-mates.
Objective Signs
Due to underlying hip muscle weakness associated with the hip joint pathology, the patient could often show poor proximal pelvic control during single position tests along with a Trendelenburg sign may be present. Passive selection of motion is going to be limited compared with the non-affected side, especially hip flexion (usually significantly less than 110°) along with hip internal rotation (less than 15°). A range of tests have been proposed that may aid the sports medicine practitioner in clinically identifying an FAI in an athlete.
Impingement Tests
FADDIR sign (22) — This evaluation involves passive hip joint flexion, adduction and internal rotation (Flexion-ADDuction- Internal Rotation). Pain is felt deeply in the anterior hip/groin region and that the assessor may sense a mechanical block to motion.
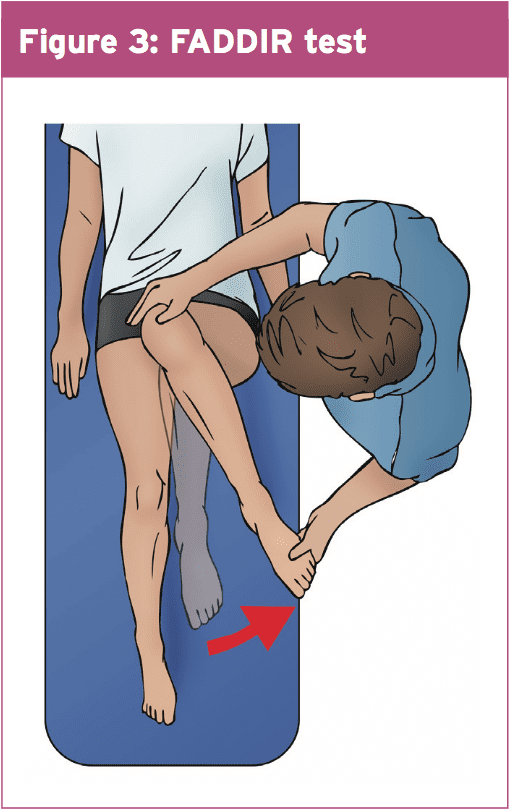
Posterior inferior impingement test(23) — With the hip in hyper expansion, passively by hanging the leg above the end of the mattress, the affected hip is passively externally rotated. The test is positive if it arouses similar pain as complained by the individual.
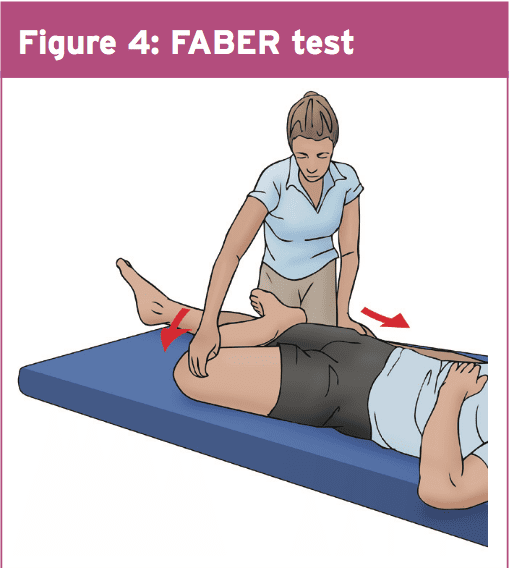
FABER test (24) — Together with the hip in flexion, abduction and external rotation (Flexion- ABDuction, External Rotation), abutment of the labrum and cartilage also can happen. The test is positive if it elicits similar pain as complained of by the patient, or when the space between the knee along with the exam table differs between the symptomatic and contra lateral hip.
Radiographs
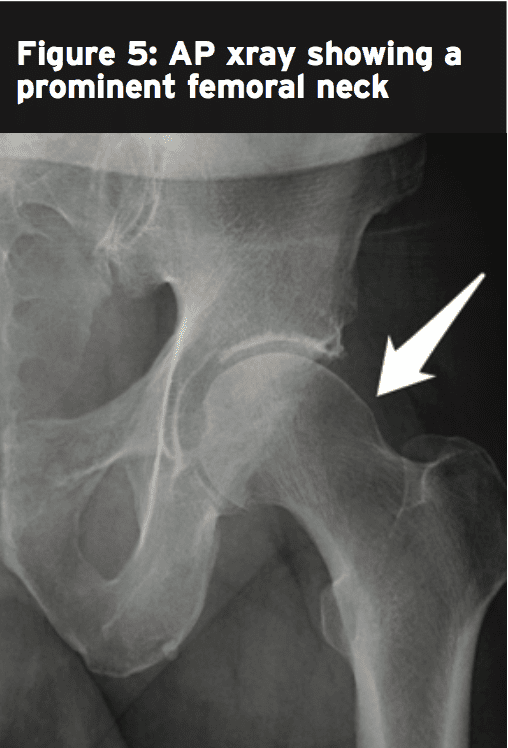
Anterior/Posterior (AP) viewpoints will also define the acetabular version like the cross- over sign. This may also be seen reminiscent of a notable anterior acetabular wall (pincer impingement). AP viewpoints will reveal acetabular retroversion, acetabular depth, os acetabulum and/or herniation pit at the neck of femur or impingement cysts can be present.
Standard Lateral View
This will identify subchondral bone sclerosis and cyst formation of the anterior acetabular rim.
Cross Table Lateral Views/Frog Lateral Views
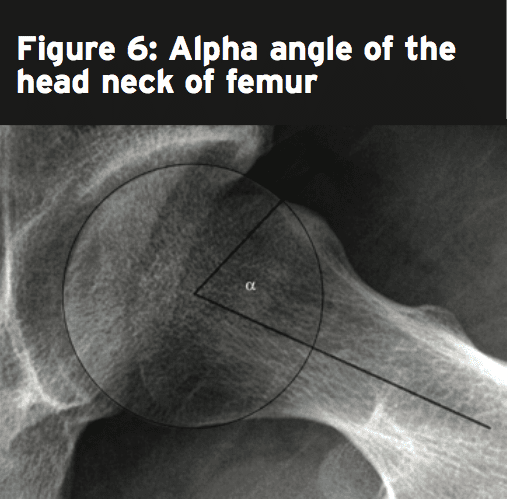
This can be completed in 10-15° internal hip rotation to compensate for femoral anteversion. This is best to view the Cam impingement lesion and reactive fibro cystic changes of the anterior head-neck junction. Other radiological measurements which can be made include head-neck offset(25), alpha angles(26), and anterior counter ratio(27).)
Magnetic Resonance Imaging (MRI) & Arthopgraphy (MRA)
MRI is helpful if hip labral pathology is suspected in conjunction with FAI, and might show articular cartilage thinning. It is more likely indicative of a subchondral stress reaction in the anterior acetabulum because of failure of the subjacent thoracic surface. Therefore, anterior acetabular subchondral edema is indicative of important articular pathology(28).
MRA is much more sensitive for seeing intra-articular pathology such as labral lesions. This can also be helpful, as the gadolinium injection related to the MRA also has local anaesthetic which can be used as a diagnostic cube to get intra-articular joint pathology.
Computerized Tomography (CT)
CT 3D reconstructions are useful to assess the shape of the femoral head neck junction and this is deemed useful for surgical resection. A new CT opinion has been invented by Pritchard and O’Donnell to show FAI lesions(29). CT scanning at the position of discomfort (POD perspective) enables symptomatic Cam deformity to be accurately mapped in a 3-dimensional reconstruction. This procedure helps in identification of the problem by visualization and following preparation for surgical resection.
Surgery
Because of the mechanical nature of FAI, conservative direction along with physiotherapy usually fails as ultimately, the impingement of bone on bone will turn out to be restrictive to the athlete. Frequently conservative applications are only effective as behaving as identifiers of both FAI and then to prevent additional mechanical symptoms by preventing the offending movements. Gym based movements such as squats past 60° hip flexion, Bulgarian squats and leg press are avoided, or modified to be done in external rotation. But, finally if pain persists then operation is the only method to handle those issues.
Before the development of more advanced hip joint surgery techniques, athletes using ‘FAI’ could have lived and performed within the confines of their symptoms. They simply would have avoided movements that generated hip joint pain and when this proved too hard to prevent, they simply would have stopped to compete. In this present day, improvements in not only diagnosis but also both open and arthroscopic hip joint operation has enabled simple management of those conditions. Therefore surgery is often recommended for your young athlete using FAI. The goal of surgery is to remove the mechanical block of the proximal femur against the acetabulum and additionally to tackle any related labral pathology and articular damage. Open and closed arthroscopic techniques are described.
 Prior to 2001, direct access into the hip joint was very difficult due to the risk of avascular necrosis, therefore most fashionable joint impingements were handled with labral debridement and/or labral reattachment. Back in 2001, Ganz et al described a surgical technique that included surgical dislocation using a ‘trochanteric reverse osteotomy’ that preserved the blood flow to the frontal brain(30). This prevented the critical negative effect of avascular necrosis of the femoral head associated with hip joint dislocation procedures. This technique led to greater diagnosis of FAI as a genuine hip joint pathology and correcting this was possible.
Prior to 2001, direct access into the hip joint was very difficult due to the risk of avascular necrosis, therefore most fashionable joint impingements were handled with labral debridement and/or labral reattachment. Back in 2001, Ganz et al described a surgical technique that included surgical dislocation using a ‘trochanteric reverse osteotomy’ that preserved the blood flow to the frontal brain(30). This prevented the critical negative effect of avascular necrosis of the femoral head associated with hip joint dislocation procedures. This technique led to greater diagnosis of FAI as a genuine hip joint pathology and correcting this was possible.
Open Surgery
This entails dislocation of the hip anteriorly using a trochanteric flap osteotomy. This allows a full view of their head neck junction. One other osseous impingement visualised can then be excised to restore the normal contour of the femoral neck fascia. Retroversion of the acetabulum may be managed with resection of the anterior acetabular rim. Any labral tear should be treated with excision or fix.
Continuing groin pain after an open process can be brought about by insufficient recovery of the femoral or acetabular morphology, advanced joint degeneration, joint space narrowing, ongoing cartilage damage, or scar adhesions between the hip joint capsule and rectal neck resection, also between the labrum and hip joint capsule(31). Whether this scarring is thick then they may interfere with movement involving the femur and acetabulum. These can impinge during flexion and internal rotation movements.
Arthroscopic Repair
Arthroscopic intervention is now becoming increasingly popular.
- Central compartment — the structures medial to the labrum.
-
Peripheral compartment the structures outside the labrum but within the hip capsule.
A traction device is utilized to separate the femur in the acetabulum to visualise the central compartment. Traction isn’t needed for peripheral compartment procedures. The joint is full of saline and also two to three portals are utilized (anterior, anterolateral or posterolateral).
The procedures achieved by hip arthroscopy presently include;
- Debridement of labral tear
- Repair of torn labrum
- Chondroplasty of acetabular lesions
- Drilling or micro fracture of acetabular lesions
- Acetabular rim excision (pincer lesions)
- Debridement of acetabular chondral delamination
- Capsular excision
- Femoral osteochondroplasty
Philippon et al (2007) discovered that at 93 percent of athletes returned to competitive sport following arthroscopically handled FAI(33). The small number who didn’t had complex OA changes at the time of surgery.
Conclusion
FAI is an increasingly more common musculoskeletal disorder affecting the young to middle aged athlete that can lead to insidious onset groin pain and harm that the hip joint labrum and lead to premature OA changes. It’s common in sports that need hip flexion and hip rotation positions as part of their art implementation. Cam and pincer lesions are the two forms of FAI lesions and these can unite to form double lesions. Conservative management generally fails in the young athlete to fully manage their pain, so surgery, either open or arthroscopic is usually the recommended treatment.
References
1. The Proceedings of the Third Open Scientific Meeting of the Hip Society. St Louis, MO: CV Mosby; 1975:212–2.
2. Ann Surg. 2008;4:656-665
3. Clin Orthop Relat Res. 2003;417:112–20
4. Clin Ortop. 1999; 363:93–9
5. Curr Rev Musculoskelet Med. 4:23–32
6. Curr Orthop. 2008;22:300–10
7. Clin Orthop Relat Res. 2010 October; 468(10): 2710–2714
8. Clin Orthop Relat Res. 2001 Dec;(393):25-37
9. Sports Health. 2014. 6(2); pp 171-177
10. Sports Health. 2014. 6(2); pp 108-118
11. J Bone Joint [Br]. 2001;83-B:171–6
12. Curr Rev Musculoskelet Med. 2009; 2: 105–117
13. Arthritis Care & Res. 2010;62 (9): 1319-1327
14. J Bone Joint Surg Am. 2010 Oct 20;92 (14):2436-44
15. Clin Orthop Relat Res. 2009;467:739-746
16. J Surg Orthop Adv. 2004;13(1):20-23
17. Radiology 2006;240(3):778-85
18. J Bone Joint Surg Br. 2005;87-B:1012–8
19. Hip Int. 2006;16(4):281-286
20. Arthritis Rheum. 2011;63 Suppl 10 :1077
21. Clin Orthop Relat Res. 2010; 468:2143–51
22. Knee Surg Sports Traumatol Arthrosc. 2007;15:1041–7
23. J Bone Joint Surg Br. 2005;87- B:1459–62
24. Clin Sports Med. 2006;25(2):299–308
25. Clin Orthop Relat Res. 2007;462:115–21
26. Clin Orthop. 2004;429:170–7
27. Hip Int. 2001;11:37–41
28. Sports Health. 2010. 2(4). pp 321-333
29. Singh PJ, PritchardM, O’Donnell J. The POD CTscan—a betterway to demonstrate FAI and early hip degeneration. Annual Scientific Meeting. International Society for Hip Arthroscopy; Oct 2009
30. The J of Bone and J Surgery. 83-B (8), pp 1119-1124
31. Clin Orthop Relat Res (2009) 467:769–774
32. Tech Orthop. 2005;20:156–62
33. Knee Surg Sports Traumatol Arthrosc (2007) 15:908–914.
Post Disclaimer
Professional Scope of Practice *
The information herein on "Hip Musculoskeletal Disorder: Femoro-Acetabular Impingement" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness, Personal Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those on this site and our family practice-based chiromed.com site, and focuses on restoring health naturally for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
Licenses and Board Certifications:
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card



 Cam Lesions
Cam Lesions Mixed Lesions
Mixed Lesions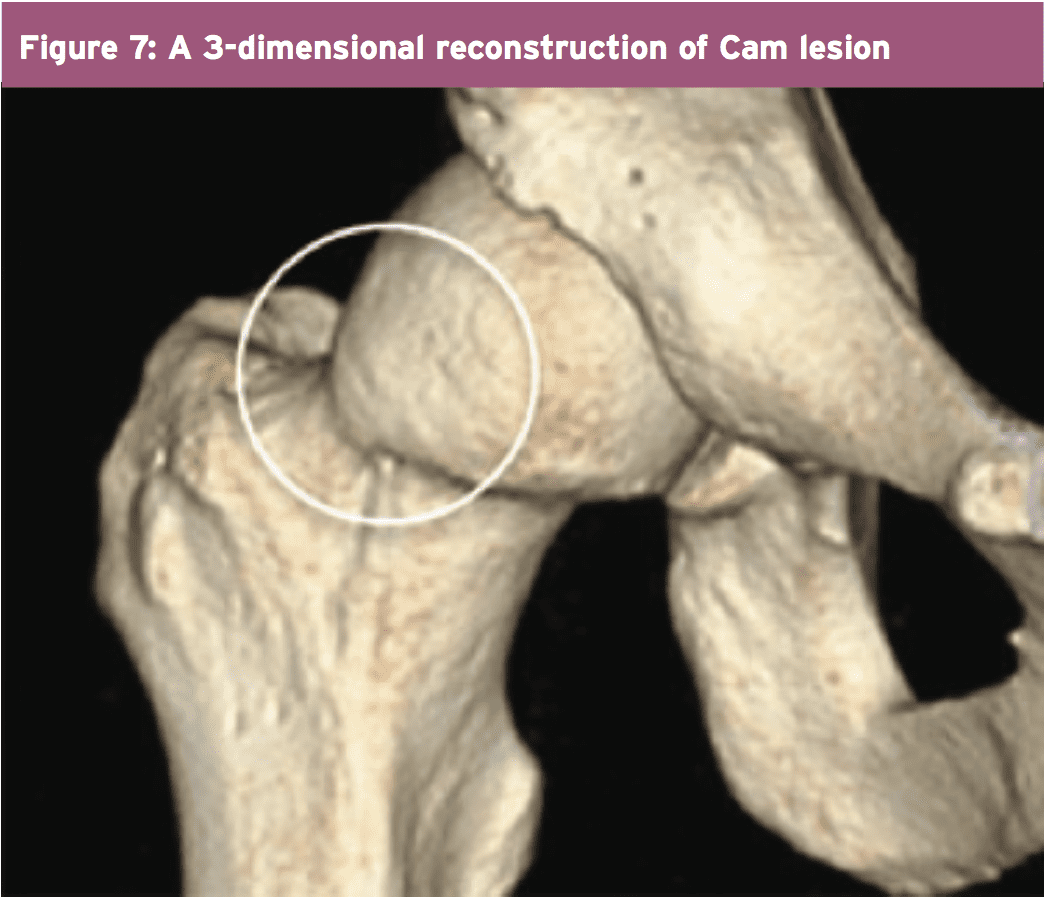


 Again, We Welcome You.
Again, We Welcome You.
Comments are closed.