A range of factors can play an essential part in the experience of chronic pain. Pain is the body’s normal reaction to an injury or illness, But for many people, pain can be a constant.
When pain lasts for 3 to 6 months or more, it’s called chronic pain. If you hurt day after day, it can take a toll on your emotional and physical health. And, if your emotional and physical health are affected, a variety of fundamental microorganisms can be affected as well. In order to maintain overall health and wellness, following a biocentric approach can often help best understand the impact of maintaining the health of every part which makes the human body. It may be beneficial to view this model to conceptualize the complex nature of this frequent condition.
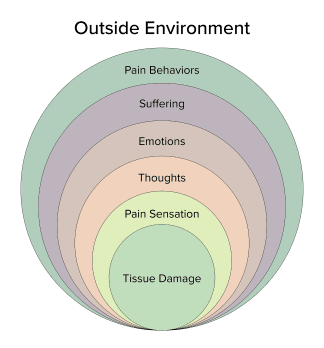
Table of Contents
Tissue Damage
This is damage or injury to the tissue which often generally can be the start of pain. The tissue damage causes input to the nervous system, commonly identified as the pain signal. This is also termed as “nociceptive input.” Each cell in the body comes together to form a variety of complex tissues, which independently come together to form organs and other important structures, each in charge of performing essential functions for the body.
Biocentrism, the view or belief that the rights and needs of humans alone are not more important than those of other living things, explains how taking care of every single structure in the body, such as the cells which form tissues, even including microorganisms, can ensure the well-being of the body as a whole. Damaged tissues can often be a sign of a deeper issue within the human body. Tissue damage can be additionally caused by a variety of other issues.
Pain Sensation
In the simplest terms of this model, pain sensation is the actual perception that occurs in the brain following the nerve signals, due to nociception, which travel from the periphery into the central nervous system. Whilst nociception occurs at the site of injury, pain sensation is experienced in the brain. The human body is not simply a single organism, it is comprised of a wide variety of microorganisms, many of which help maintain the well-being of the nervous system.
Thoughts
Cognitions or ideas occur and are an assessment of the pain sensation signal coming into the nervous system as well as events surrounding it. These thoughts can be unconscious or conscious and will influence the way pain signals are perceived. For example, general body aches and stiffness are traditionally considered to be “good pain” when those happen after a vigorous exercise session, whereas they’re perceived as bad pain when related to a health illness, such as fibromyalgia, a chronic disorder characterized by widespread musculoskeletal pain, fatigue, and tenderness.
Emotions
The psychological component of pain is a person’s response to thoughts about the pain. If you believe (thoughts) that the pain is a serious danger (e.g. a tumor), subsequently emotional responses will incorporate fear, depression, and anxiety, amongst others. If you believe the pain isn’t a threat, then the psychological response will probably be negligible. Chronic pain has been a misunderstood condition and it’s effects have been reported to cause an array of emotional as well as mental disorders, due to the difficult ability to assess such conditions.
Suffering
The term “suffering” is often employed as a synonym for “pain” even though they’re theoretically and conceptually distinct. For example, a broken bone might cause pain without discomfort (since the individual knows the pain isn’t deadly and the bone will heal). By comparison, bone pain due to a tumor might cause the identical pain for a break but the distress will be much greater because of the “meaning” behind the pain (that tumor could be life-threatening). Suffering is connected to the psychological component of pain. For certain conditions which cause chronic pain, often seen in patients with fibromyalgia, a condition believed to have no cure, the fact alone that the individual’s symptoms of discomfort will never “go away” can implement a great deal of suffering.
Pain Behaviors
Pain behaviors are defined as things people do if they are in pain or suffer. These are behaviors that others observe as indicating pain, like limping, grimacing, talking about the pain, moving and taking pain medication. Pain behaviors are in reaction to all the other facets in the pain system model (tissue damage, pain feeling, thoughts, emotions, and distress). Life experiences, expectations, and ethnic influences also affect pain behaviors of the way the pain is expressed in terms. Interestingly, pain behaviors are also influenced by the environment, like how others react.
According to biocentrism, taking care of the environment, including taking care of all forms of life, such as its plants and animals, among others, is ultimately important towards the health and wellness of every organism. For example, if the food we eat is being properly taken care of, its full benefits can be properly absorbed. Nutrition is an important contributing factor for people with chronic pain. A balanced nutrition, consisting of healthy products, can help.
Additionally, the psychosocial environment includes each of the environments where an individual resides, works, and plays. Studies have consistently proven that these surroundings influence how an individual will reveal pain behaviors.
The scope of our information is limited to chiropractic and spinal injuries and conditions. To discuss options on the subject matter, please feel free to ask Dr. Jimenez or contact us at 915-850-0900 . 
By Dr. Alex Jimenez
Additional Topics: Wellness
Overall health and wellness are essential towards maintaining the proper mental and physical balance in the body. From eating a balanced nutrition as well as exercising and participating in physical activities, to sleeping a healthy amount of time on a regular basis, following the best health and wellness tips can ultimately help maintain overall well-being. Eating plenty of fruits and vegetables can go a long way towards helping people become healthy.

TRENDING TOPIC: EXTRA EXTRA: New PUSH 24/7Â®ï¸ Fitness Center
Post Disclaimer
Professional Scope of Practice *
The information herein on "Understanding Chronic Pain | Chiropractic Care Clinic" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness, Personal Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those on this site and our family practice-based chiromed.com site, and focuses on restoring health naturally for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
Licenses and Board Certifications:
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card





 Again, We Welcome You.
Again, We Welcome You.
Comments are closed.