Enhance your knowledge of therapeutic approaches to tissue regeneration using photobiomodulation and its role in advanced healing therapies.
Table of Contents
Abstract
This educational post guides clinicians and patients through a modern, evidence-based approach to managing low back pain, joint stiffness, trigger points, and post-procedural recovery using multiwave locked system (MLS) laser therapy in an integrative chiropractic care model. Drawing on the latest peer-reviewed research and clinical observations from my practice, I explain how precise dosing via energy density (4–10 J/cm²), dual-wavelength pulsed delivery, and robotic targeting improve outcomes while maintaining patient comfort. I detail why MLS laser therapy can modulate pain signaling, inflammation, microcirculation, mitochondrial bioenergetics, and tissue healing without inducing excessive thermal load. I also present practical protocols for combining MLS laser with orthobiologics (e.g., PRP), shockwave therapy, targeted exercise, and manual chiropractic methods. Specific attention is given to safe dosing, workflow, acute and chronic pathways of biological change, and optimization strategies using nutrition and lifestyle. By the end, you will understand how and why we aim for density over total joules, how software-guided XY field changes auto-recalculate treatment time, and how integrative chiropractic care coordinates robotics and handpiece strategies to address the pain generator and its kinetic chain.
Patient Comfort and Precision Targeting in MLS Laser Therapy
In my clinical experience, patient comfort is the first step to an effective laser session. When we position a patient—especially for low back work—we typically place them prone, allowing direct contact with the skin and ensuring optimal photon delivery without fabric interference. With robotic MLS laser systems, stability matters: we align the beam carefully over the symptomatic area so the patient can remain still. This reduces motion artifacts and keeps the dose consistent.
- Key comfort measures:
-
- Face-down positioning for lumbar applications
- Direct-to-skin contact when using the handpiece for focal dosing
- Cushioned bolsters and neutral-spine support to reduce movement
- Coaching and check-ins during the session to maintain alignment
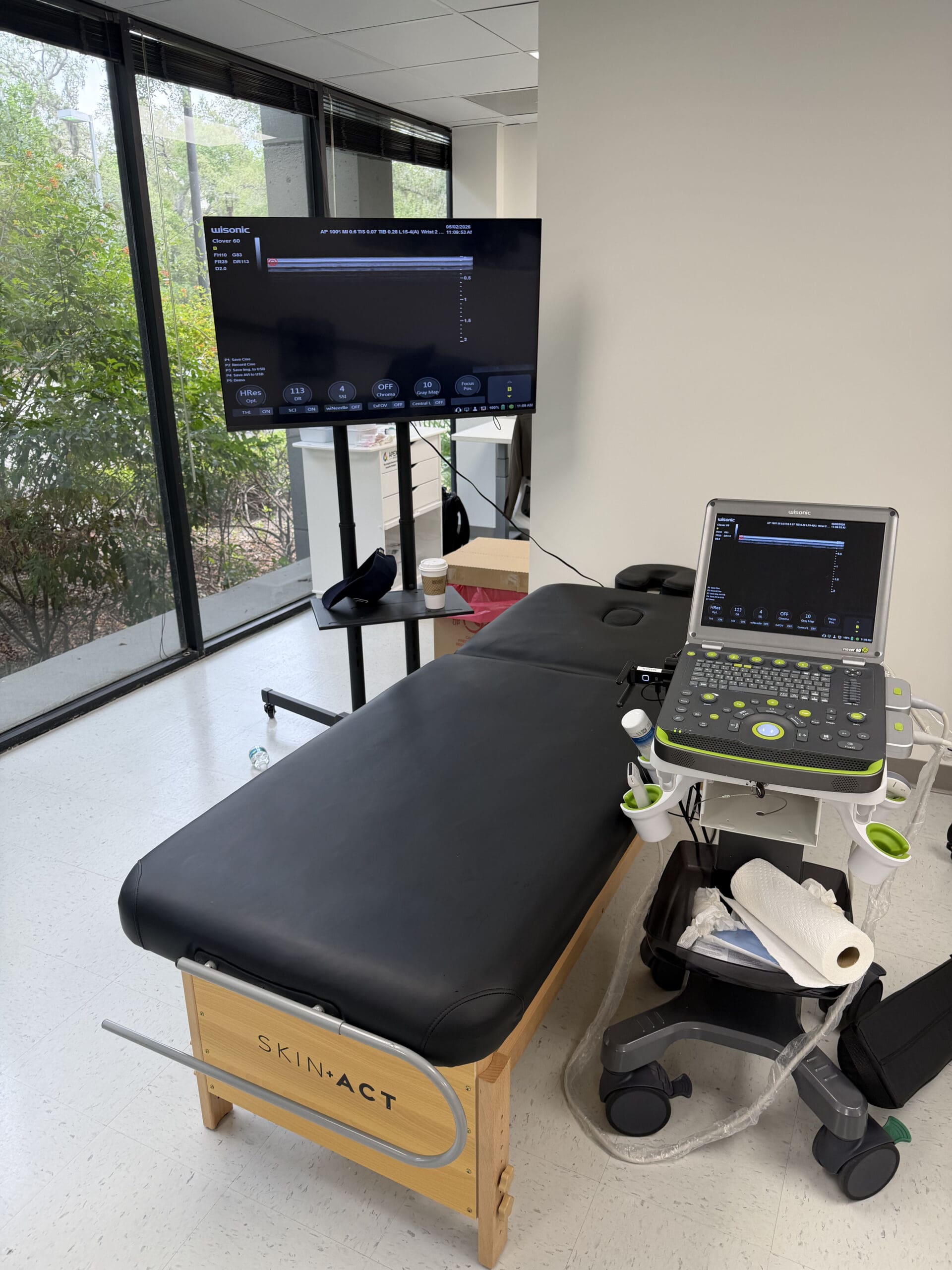 From a workflow perspective, I first center the beam over the patient’s primary pain generator (e.g., facet-mediated pain around L4–L5) and then expand the X and Y fields to encompass the painful area and adjacent connective tissues. This is part of a clinical multimodal approach in which we treat the source and the surrounding myofascial network. Modern MLS robotics provides ruler-guided standoff distances—typically about six inches—so we maintain an accurate focal point. The beam is collimated, giving slight latitude in depth and field uniformity, but precise setup yields the most consistent outcomes.
From a workflow perspective, I first center the beam over the patient’s primary pain generator (e.g., facet-mediated pain around L4–L5) and then expand the X and Y fields to encompass the painful area and adjacent connective tissues. This is part of a clinical multimodal approach in which we treat the source and the surrounding myofascial network. Modern MLS robotics provides ruler-guided standoff distances—typically about six inches—so we maintain an accurate focal point. The beam is collimated, giving slight latitude in depth and field uniformity, but precise setup yields the most consistent outcomes.
Why this matters physiologically:
- Photonic energy must reliably reach target chromophores (e.g., cytochrome c oxidase) to trigger mitochondrial responses that increase ATP production and modulate reactive oxygen species (ROS) within therapeutic ranges.
- Stable targeting improves microvascular perfusion and lymphatic drainage, reducing edema and nociceptive input from inflamed periarticular tissues.
Robot vs. Handpiece: Two Channels, One Integrative Strategy
I commonly pair the robotic emitter with a direct-contact handpiece for combined coverage. The robot, equipped with multiple diodes and dual wavelengths, delivers a uniform dose over a shaped field (e.g., a triangular footprint visible as an 808 nm area in camera images). The handpiece has a single diode designed for direct skin contact and for precise trigger-point or joint-line applications.
- Robot channel:
-
- Dual wavelengths (typically 808 nm continuous/pulsed and 905 nm superpulsed)
- Auto-calculated dosing when the XY field size changes
- Best for larger regions, post-surgical fields you prefer not to touch, or non-contact needs
- Handpiece channel:
-
- Direct, punctual dosing for trigger points, joint spaces, and dynamic movement during treatment
- Ideal when you want patient-assisted motions to recruit the kinetic chain while you stimulate focal tissues
- Useful for nerve pain or sensitized areas where fine control is needed
Clinical reasoning:
- Combining channels lets me address the primary pathology while recruiting adjacent myofascial chains and neuromuscular patterns that perpetuate pain.
- A focal handpiece can “de-knot” hypertonic loci—the proverbial cooked-meat feel compared to soft, raw muscle—while the robot maintains steady regional anti-inflammatory and circulatory effects.
Dose Fundamentals: Energy Density Over Total Joules
A frequent point of confusion is dose quantification. We prioritize energy density (J/cm²) rather than absolute total joules. The target therapeutic window commonly cited in laser therapy literature is 4–10 J/cm², adjusted by condition and tissue depth. In practice, I often use ~6 J/cm² for lumbar facet and myofascial pain, then track the total joules as a function of area to ensure the density remains on target.
- Why density matters:
-
- Tissue responses follow dose-dependent biological laws (e.g., the Arndt-Schulz principle), meaning that too little energy fails to provoke a response, while too much can yield bioinhibition.
- Density controls for area, so a changed XY field doesn’t accidentally overdose or underdose the region.
- Modern MLS software recalculates treatment time automatically when the XY field is resized, preserving the desired J/cm².
Physiology at play:
- The right energy density supports ATP synthesis, nitric oxide signaling, and controlled ROS formation, which together drive improved microcirculation, pain modulation, and cell signaling for repair.
- By staying in the therapeutic window, we avoid excessive surface heating and promote stronger photonic effects without tissue stress.
Pulse Dynamics, Power, and Tissue Safety
MLS laser systems merge high peak power—often up to 50 W in superpulsed modes—with short pulse durations and dual wavelengths to deliver energy without overheating tissues. The 905 nm superpulsed beam penetrates deeply thanks to short bursts of high intensity, while the 808 nm wavelength contributes steady energy that cameras can sometimes visualize as a triangular footprint. Both wavelengths pulse in coordination, followed by brief rest intervals that allow energy absorption and thermal diffusion, keeping tissue temperatures steady over time.
- Clinical takeaway:
-
- If the patient feels significant surface heat, the wavelength or dose is likely wrong, or the tissue cannot absorb the delivered energy at that pace.
- Properly tuned MLS ensures constant tissue temperature, signaling safe and effective energy transfer.
Physiological rationale:
- Short, high-intensity pulses drive photobiomodulation into deeper tissues while limiting thermal accumulation.
- Rest intervals favor photon–chromophore interaction without exceeding local thermal thresholds, protecting superficial structures and peripheral nociceptors.
Acute vs. Chronic: Understanding the Biological Cascade
Patients often ask why the MLS laser can help both acute pain and chronic degeneration. The answer lies in the layered physiology:
- Acute phase (first hours to days):
-
- Fast pain modulation through effects on small myelinated fibers, reduced nociceptive signaling, and early microcirculatory changes
- Edema reduction via improved lymphatic flow
- Subtle thermogenic comfort without damaging heat
- Subacute progression (days to weeks):
-
- Inflammatory modulation with downregulation of pro-inflammatory cytokines and upregulation of anti-inflammatory mediators
- Enhanced angiogenesis and fibroblast activity toward repair
- Mitochondrial optimization—balanced ROS, increased ATP, improved cellular respiration
- Chronic remodeling (weeks to months):
-
- Support for collagen alignment, tendon remodeling, and myofascial normalization
- Reduced central sensitization drivers through sustained peripheral calm
- Improved functional biomechanics, especially when combined with chiropractic adjustments, targeted exercise, and shockwave for tendinopathies
We cannot selectively “turn on” only one effect—pain modulation, inflammation control, or mitochondrial enhancement—because they are interdependent. Instead, we sequence protocols by clinical goals, tuning frequency sets, pulsing, and field size to emphasize relevant outcomes during each stage.
Integrative Chiropractic Care: Coordinating Laser, Manual Therapy, and Movement
MLS laser fits naturally within integrative chiropractic care, where we combine manual adjustments, soft-tissue release, corrective exercise, neuromuscular re-education, and, when appropriate, orthobiologics. My clinical observations, shared across cases on ChiropracticScientist.com and LinkedIn, underscore that laser therapy enhances the efficacy of:
- Facet arthropathy and lumbar paraspinal hypertonicity:
-
- Laser reduces local inflammation and muscle guarding
- Chiropractic adjustments restore segmental motion, while exercise reinforces motor control
- Trigger points and myofascial pain:
-
- Handpiece dosing to focal knots, paired with myofascial release and breathing cues
- Robot covers the broader region to optimize circulation and neuromodulation
- Knee osteoarthritis:
-
- Treat in flexion to reduce patellar reflection and reach deeper joint spaces
- Address medial and lateral compartments individually by maintaining correct J/cm² per field
- Combine with shockwave for tendinopathy, exercise therapy for strength and alignment, and weight management strategies
Why integration amplifies results:
- Laser prepares tissues by improving perfusion and cell signaling, making them more responsive to manual input.
- Adjustments and mobilizations then recalibrate joint mechanics, which reduces ongoing nociceptive drive.
- Exercise consolidates gains by retraining stability, coordination, and load tolerance.
Practical Protocols: Acute, Chronic, and Orthobiologics Synergy
In acute conditions, I recommend six MLS sessions spaced by at least 24 hours (e.g., Monday-Wednesday-Friday schedules). Chronic conditions generally require 12 sessions in similar spacing to build cumulative effects. Patients often begin feeling better after 3–5 sessions, but completing the prescribed series prevents relapse and supports long-term remodeling.
- Acute pain:
-
- 6 sessions within 2–3 weeks
- Emphasis on pain modulation, edema control, and early mobility restoration
- Chronic pain or degeneration:
-
- 12 sessions over 4–6 weeks
- Emphasis on inflammation control, mitochondrial support, and functional retraining
- Orthobiologics (e.g., PRP) integration:
-
- 2–3 MLS sessions before injection to prime the target tissue and improve the microenvironment
- 1 session on the day of injection with settings that support perfusion and comfort without suppressing desired early inflammation
- About 6 sessions post-injection to sustain repair signaling and reduce pain, enhancing outcomes relative to PRP alone
Clinical note:
- Post-injection strategies should respect the pro-inflammatory phase of PRP (typically 7–10 days). Proper MLS parameters can augment rather than blunt regenerative signaling, improving overall cellular responsiveness and tissue perfusion.
Off-Label Considerations: Bone Healing Windows
While bone healing assisted by laser therapy is frequently discussed, it is often considered off-label in many jurisdictions. Clinically, I have observed potential benefits in the early inflammatory phase of fracture healing—particularly when initiated within 7–10 days—to support local circulation and cellular activity. Non-unions are more complex and typically demand comprehensive management strategies, such as PRP, bone stimulators, or surgical consultation. Transparent communication with patients is essential: laser may be one piece of a larger strategy, not a standalone solution for structural deficits.
Avoiding Overdose: Bioinhibition and Field Stacking
The body can absorb and utilize only a finite amount of photonic energy at a single site at a time. When patients ask for “more time” at a single location, I recommend field stacking—treating the anterior and posterior or medial and lateral compartments—while preserving the therapeutic J/cm² per field, rather than simply extending time at one spot. This reduces the risk of bioinhibition (too much stimulation leading to diminished effects) and spreads benefits across the functional unit.
Visualizing the Dose: What Your Phone Shows
Patients enjoy seeing the therapy footprint. The camera can detect the 808 nm wavelength as a geometric pattern (often triangular) representing the treated area. The 905 nm component, delivered in superpulses, typically isn’t visible on consumer cameras due to its pulse characteristics. This visualization helps patients understand that dose is not the entire “red hue” but rather the defined beam footprint, reinforcing why alignment and stillness matter.
Comfort Sensations and Sensitivity
Most patients feel little to no sensation during MLS therapy. Sensitive patients may describe mild warmth or light tingling, which is normal and can be reframed positively. With dual-wavelength pulsing and proper density control, we rarely encounter excessive heat. If a patient feels notable warmth, reassess distance, field size, settings, and contact method (robot vs. handpiece).
Knee Osteoarthritis: Density-Driven Compartment Care
For knees, I determine the primary compartments (medial, lateral, posterior) based on symptoms and imaging. The patella can reflect a significant portion of the incident energy when the knee is extended; it’s better to treat in flexion, allowing deeper penetration into the joint. I apply 6–8 J/cm² per compartment rather than arbitrarily increasing the total joules. If space is severely narrowed, MLS can help with pain and inflammation but will not restore cartilage in end-stage bone-on-bone conditions; we then focus on multimodal pain control, load management, and surgical consultation as indicated.
Mitochondrial Optimization: Nutrition, Lifestyle, and Medications
Laser-induced photobiomodulation supports mitochondrial function by engaging cytochrome c oxidase, increasing ATP production, modulating ROS levels, and influencing downstream gene expression related to repair. To optimize these effects:
- Supportive strategies:
-
- Creatine for phosphate donation to buffer ATP demands
- Coenzyme Q10 and NAD precursors to enhance electron transport
- Polyphenols and omega-3s for inflammation and membrane health
- Sleep, glycemic control, and aerobic base training to improve mitochondrial biogenesis
- Medication considerations:
-
- Some statins and metformin can influence mitochondrial pathways. Coordination with prescribers is vital; we do not advise unilateral changes. Instead, we individualize care and monitor function and symptoms, leveraging lasers to support bioenergetics as part of a safe medical plan.
This holistic approach minimizes metabolic friction and lets MLS-induced mitochondrial cues translate into clinically meaningful improvements.
Reliability, Maintenance, and Field Service Support
High-quality MLS systems are robust. The primary risk point is shipping—these devices arrive in protective crates and require on-site installation and training. In my experience, ongoing reliability is strong, and manufacturers often provide field service to avoid re-shipping, lowering the risk of transport damage. Proper usage, dust protection, and scheduled checks keep the system functioning optimally for years.
Exploring Integrative Medicine- Video
Outcome Expectations and Timing
Pain does not emerge in ten minutes, and it rarely disappears permanently in ten minutes. With MLS, expect:
- Initial changes within hours: many patients notice improved comfort 4–6 hours post-session. If we meet on 2026-05-02 at 11:00, I ask patients to reassess around 17:00 on 2026-05-02.
- Early functional gains after several sessions: significant improvements often appear by the third to fifth session.
- Cumulative benefits by completing the series: finishing 6–12 sessions stabilizes changes and supports lasting function.
We coordinate with patients to avoid premature discontinuation as they start feeling better; completing the plan ensures durability.
Case-Guided Application: Low Back Pain with Facet Involvement
For a patient describing joint pain and stiffness with likely facet involvement at L4–L5, plus intermittent radiation to the right, I:
- Position prone for skin contact and comfort.
- Center the robotic footprint over the pain generator.
- Expand XY to include adjacent paraspinals and thoracolumbar fascia.
- Dose at ~6 J/cm² for 8 minutes, with auto time adjustment based on field size.
- Use the handpiece for focal trigger points, applying ~6–8 J/cm² at each site in quick 20–30-second intervals.
- Follow with gentle mobilization, segmental adjustments if indicated, and breathing-based core activation.
- Integrate gluteal strength, hip hinge mechanics, and lumbopelvic motor control to reduce facet loading.
This sequence reduces nociception, normalizes muscle tone, and restores segmental motion, aligning with the physiologic cascade described above.
Putting It All Together: A Modern, Evidence-Based Pathway
- Start with patient comfort and precise targeting.
- Favor energy density over total joules; leverage auto-calculations when changing field size.
- Combine robotic regional dosing with handpiece focal work.
- Sequence care across acute, subacute, and chronic phases with complementary chiropractic and exercise
- Integrate with orthobiologics using pre-, day-of, and post-injection protocols that augment rather than blunt biologic intent.
- Optimize mitochondrial and inflammatory environments with lifestyle and nutrition, in coordination with medical prescribers.
This integrative approach reflects current research trajectories and aligns with outcomes I observe in practice: improved pain control, better function, and a smoother recovery arc.
In-Text Citations
- The importance of energy density (4–10 J/cm²) and photobiomodulation dose windows has been articulated in consensus statements and meta-analyses in the laser therapy literature (e.g., the World Association for Laser Therapy guidelines).
- Dual-wavelength, superpulsed delivery for deeper penetration with thermal safety is supported by photobiomodulation research that details mitochondrial activation via cytochrome c oxidase and dose-dependent modulation of ROS (Hamblin, 2017; Karu, 1999).
- Integrative protocols combining laser therapy with orthobiologics demonstrate additive benefits in pain reduction and functional recovery when dosing respects biologic phases (Andia & Maffulli, 2017; Fitzpatrick et al., 2017).
- Chronic musculoskeletal care benefits from multimodal strategies including chiropractic adjustments, exercise therapy, and photobiomodulation (Hurwitz et al., 2018; Bjorland et al., 2021).
References
- World Association for Laser Therapy (WALT) Guidelines (n.d.). Photobiomodulation dosing and clinical recommendations.
- Hamblin, M. R. (2017). Mechanisms and applications of the anti-inflammatory effects of photobiomodulation. Photobiomodulation, Photomedicine, and Laser Surgery.
- Karu, T. (1999). Primary and secondary mechanisms of action of visible to near-IR radiation on cells. Journal of Photochemistry and Photobiology B: Biology.
- Andia, I., & Maffulli, N. (2017). Platelet-rich plasma for managing pain and inflammation in osteoarthritis. Orthopedic Reviews.
- Fitzpatrick, J., Bulsara, M., McCrory, P., Richardson, M., & Zheng, M. H. (2017). Analysis of platelet-rich plasma efficacy for osteoarthritis through placebo-controlled studies. The American Journal of Sports Medicine.
- Hurwitz, E. L., Kominski, G. F., & Morgenstern, H. (2018). Chiropractic care and health outcomes among older adults with chronic musculoskeletal pain. Spine.
- Bjorland, S., et al. (2021). Photobiomodulation for musculoskeletal pain: A systematic review and meta-analysis. Scientific Reports.
For more of my clinical observations and case insights, visit:
SEO tags: MLS laser therapy, photobiomodulation, chiropractic care, low back pain, facet joint pain, trigger points, energy density, J/cm² dosing, dual wavelength laser, superpulsed laser, PRP integration, orthobiologics, mitochondrial optimization, pain modulation, inflammation reduction, microcirculation, shockwave therapy, knee osteoarthritis, manual therapy integration, robotic laser therapy
Post Disclaimer
Professional Scope of Practice *
The information herein on "Therapeutic Approaches Overview for Tissue Regeneration with Photobiomodulation" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness, Personal Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those on this site and our family practice-based chiromed.com site, and focuses on restoring health naturally for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
Licenses and Board Certifications:
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card




 Again, We Welcome You.
Again, We Welcome You.
Comments are closed.