These assessment and treatment recommendations represent a synthesis of information derived from personal clinical experience and from the numerous sources which are cited, or are based on the work of researchers, clinicians and therapists who are named (Basmajian 1974, Cailliet 1962, Dvorak & Dvorak 1984, Fryette 1954, Greenman 1989, 1996, Janda 1983, Lewit 1992, 1999, Mennell 1964, Rolf 1977, Williams 1965).
Table of Contents
Clinical Application of Neuromuscular Techniques: Medial Hamstrings and Adductors
Assessment for shortness in medial hamstrings (semi-membranosus and semi-tendinosus as well as gracilis) and short adductors (pectineus, adductors brevis, magnus and longus)
Method (a) The patient lies so that the non-tested leg is abducted slightly, heel over the end of the table. The leg to be tested is close to the edge of the bed and the practitioner ensures that the tested leg is in its anatomically correct position, knee in full extension and with no external rotation of the leg, which would negate the test.
The practitioner should effectively stand between patient’s leg and the table so that all control of the tested leg is achieved with his lateral (non-table-side) arm/hand, while the table-side hand can rest on and palpate the inner thigh muscles for sensations of bind as it is taken into abduction. Abduction of the tested leg is introduced passively until the first sign of resistance is noted (see Fig. 4.3). Effectively, there are three indicators of this resistance:
- A sense that the motive hand carrying the leg picks up as an increase in required effort at the moment that the first resistance barrier is passed
- The sense of bind noted by the palpating hand at this same moment
- A visual sign, movement of the pelvis as a whole, laterally towards the tested side, as the barrier is passed.
If abduction produces an angle with the mid-line of 45° or more, then no further test is needed, the abduction is normal, and there is probably no shortness in the short or long adductors (medial hamstrings or, more correctly, gracilis and biceps femoris). If, however, abduction ceases before a 45° angle is easily achieved (without effort or a sense of bind in the tissues), then restriction exists in either the medial hamstrings or the short adductors of the thigh.
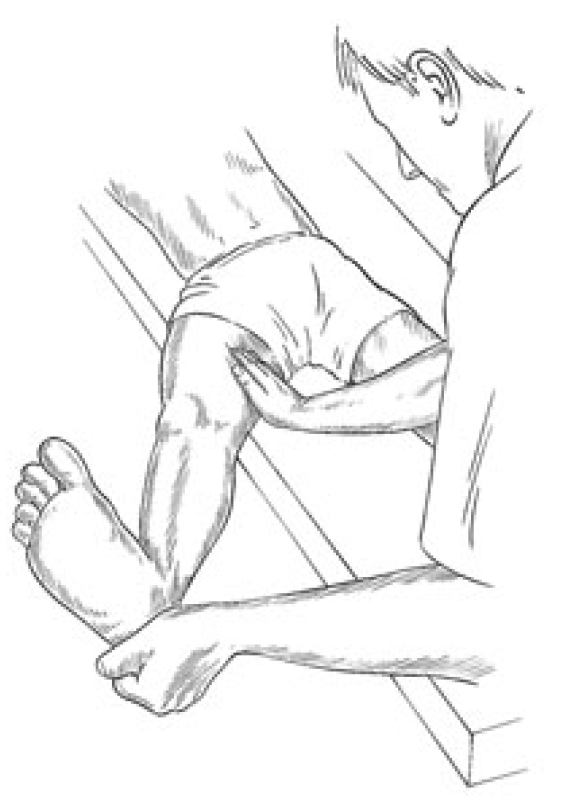
Figure 4.3 Assessment and treatment position for medial hamstrings. Adductor shortness may be evaluated and treated in the same relative position but with the knee of the leg to be treated in flexion.
Screening Short Adductors from Medial Hamstrings
As in the tests for gastrocnemius and soleus, it is necessary to screen between shortness of the one and two joint muscles (in this case the short adductors and the medial hamstrings). This is achieved by abducting the leg to its easy barrier and then introducing flexion of the knee, allowing the lower leg to hang down freely.
If (after knee flexion has been introduced) further abduction is now easily achieved to 45°, this indicates that any previous limitation into abduction was the result of medial hamstring shortness, since this is no longer operating once the knee has been flexed. If, however, restriction remains (as evidenced by continued ‘bind’ or obvious restriction in movement towards allowing a 45° excursion once knee flexion has been introduced to the abducted leg), then it is apparent that the short adductors are continuing to prevent movement, and are short.
Assessing for shortness in medial hamstring (03) /short adductors (04)
Method (b) The patient lies at the very end of table (coccyx close to edge), non-tested leg fully flexed at hip and knee and held to chest by patient (or sole of patient’s foot resting against practitioner’s lateral chest wall) to stabilise pelvis in full rotation, so that the lumbar spine is not in extension. Tested leg is grasped both above and below the knee and taken into abduction to the first sign of resistance. The practitioner has two free hands in this position, one of which can usefully palpate the inner thigh for bind during the assessment.
If abduction reaches 45°, then the test has revealed no shortness. If a restriction/resistance barrier is noted before 45°, then the knee should be flexed to screen the short adductors from the medial hamstrings as in method (a) above. In all other ways the findings are interpreted as above.
MET Treatment of Shortness in Short and Long Adductors of the Thigh
Precisely the same positions may be adopted for treatment as for testing, whether test method (a) or test method (b) was used. If the short adductors (pectineus, adductors brevis, magnus and longus) are being treated, then the leg, with knee flexed, is held at the barrier (acute) or a little short of the barrier (chronic).
An isometric contraction is introduced by the patient using around 20% of available strength (longer and somewhat stronger for chronic than acute) employing the agonists (the push is away from the barrier of resistance) or the antagonists (the push is towards the barrier of resistance) for 7–10 seconds. Appropriate breathing instructions should be given (see notes on breathing in Box 4.2).
After the contraction ceases and the patient has relaxed, the leg is eased to its new barrier (if acute) or painlessly (assisted by the patient) beyond the new barrier and into stretch (if chronic), where it is held for not less than 10 seconds (longer if possible), in order to stretch shortened tissue. The process is repeated at least once more.
If the medial hamstrings (semi-membranosus, semi-tendinosus as well as gracilis) are being treated, all elements are the same, except that the leg should be held in extension, with no bend of the knee (Fig. 4.4).
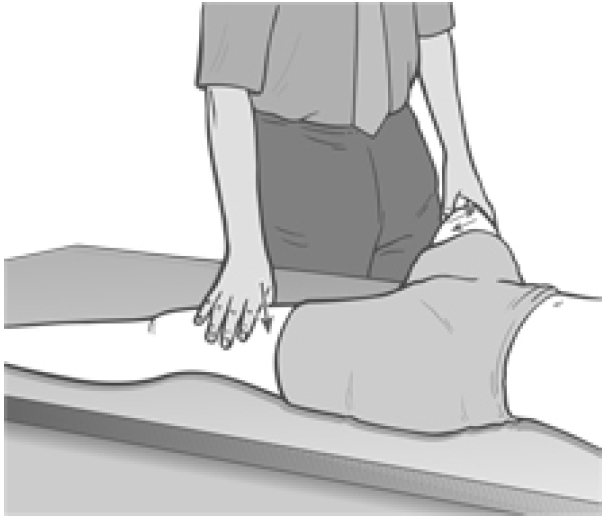
Figure 4.4 Position for treatment of shortness in adductors of the thigh.
Whichever position is used, the subsequent stretch, on an exhalation, is used to (acute) or through (chronic) the barrier to commence normalisation of the short muscles.
Caution and Alternative Treatment Position (Fig. 4.5)
The major error made in treating these particular muscles using MET relates to allowing a pivoting of the pelvis and a low spinal sidebend to occur. Maintenance of the pelvis in a stable position is vital, and this can most easily be achieved via suitable straps or, during treatment, by having the patient side-lying with the affected side uppermost.
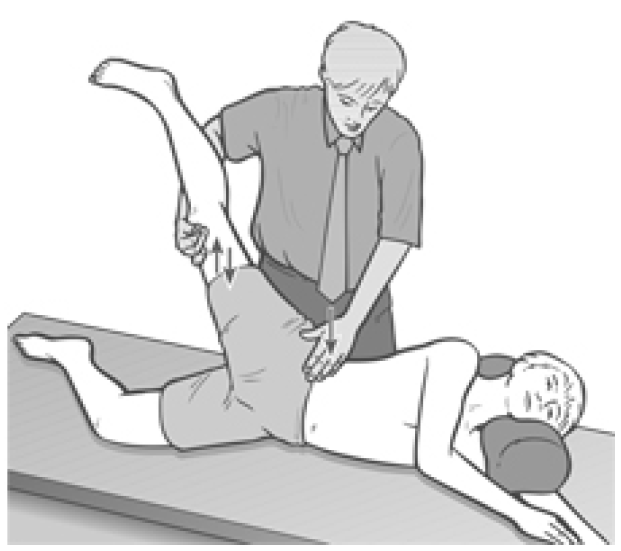
Figure 4.5 Sidelying position for treatment of two-joint adductors of the thigh.
Method (c) Patient is side-lying. Practitioner stands behind and uses the caudad arm and hand to control the leg and to palpate for bind, with the treated leg flexed or straight as appropriate. The cephalad hand maintains a firm downwards pressure on the lateral pelvis to ensure stability during stretching. All other elements of treatment are identical to those described for supine treatment above.
Dr. Alex Jimenez offers an additional assessment and treatment of the hip flexors as a part of a referenced clinical application of neuromuscular techniques by Leon Chaitow and Judith Walker DeLany. The scope of our information is limited to chiropractic and spinal injuries and conditions. To discuss the subject matter, please feel free to ask Dr. Jimenez or contact us at 915-850-0900 .
By Dr. Alex Jimenez

Additional Topics: Wellness
Overall health and wellness are essential towards maintaining the proper mental and physical balance in the body. From eating a balanced nutrition as well as exercising and participating in physical activities, to sleeping a healthy amount of time on a regular basis, following the best health and wellness tips can ultimately help maintain overall well-being. Eating plenty of fruits and vegetables can go a long way towards helping people become healthy.

ADDITIONAL TOPIC: EXTRA EXTRA: Treating Back Pain
Post Disclaimer
Professional Scope of Practice *
The information herein on "Assessment and Treatment of Medial Hamstrings and Adductors" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness, Personal Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those on this site and our family practice-based chiromed.com site, and focuses on restoring health naturally for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
Licenses and Board Certifications:
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card





 Again, We Welcome You.
Again, We Welcome You.
Comments are closed.