El Paso, TX. Chiropractor Dr. Alex Jimenez looks at types of treatments for Plantar Fasciitis
Plantar fasciitis: a condition in which weight-bearing stress irritates and inflames the tough connective tissues along the bottom of the foot. Like stated by Mary Biancalana  Plantar Fasciitis? Maybe Not, So Don’t Ice It!, most often, when pain is felt in the bottom of the foot, it is instantly diagnosed as plantar fasciitis. Since it is important to get an accurate diagnosis, it is important to correctly diagnose plantar fasciitis before treating. So, have you been properly diagnosed? Let’s learn more and how to treat plantar fasciitis!
Table of Contents
Pathology
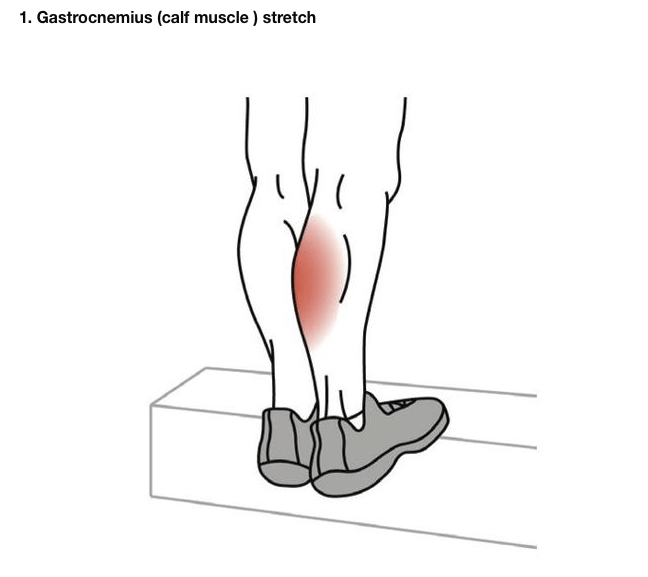
Plantar fasciitis develops when repetitive weight-bearing stress irritates and inflames the tough connective tissues along the bottom of the foot. High levels of strain stimulate the apo-neurosis to try to heal and strengthen. When the biochemical strain continues, it overwhelms the body’s repair capacity, and the ligaments begin to fail. This tear/repair process causes the chronic, variable symptoms that eventually can become unbearable for some patients.
Since the plantar fascia inserts into the base of the calcaneus, the chronic pull and inflammation can stimulate the deposition of calcium, resulting in a classic heel spur seen on a lateral radiograph. Unfortunately, there is no correlation between the resence of a heel spur and plantar fasciitis, since many heel spurs are clinically silent, and most cases of plantar fasciitis do not demonstrate a calcaneal spur. 1
Examination
Biomechanical evaluation may find either excessive pronation or supination. The flatter, hyperpronating foot overstretches the bowstring function of the plantar fascia, while the high-arched rigid foot places excessive tension on the plantar aponeurosis. In either case, the combination of improper foot biomechanics and excessive strain causes the connective tissue to become inflamed. A careful assesment of the weight bearing alignment of the lower extremeties is helpful, since many patients will have funactional imbalances in the kinetic chain, into the pelvis and spine.
Direct palpation of the plantar fascia will demonstrate discrete painful areas, most commonly at the insertion on the anterome-dial calcaneus.2 Â Fibrotic thickenings are frequently felt- these are remants of the repetitive tear and repair process. With the foot relaxed, grasp the toes and gently pull them up into passive dorsiflexion. Since this maneuver stretches the irritated plantar aponeurosis, it is frequently quite painful, which is an obviously positive objective sign.
Treatment
Acute ReliefÂ
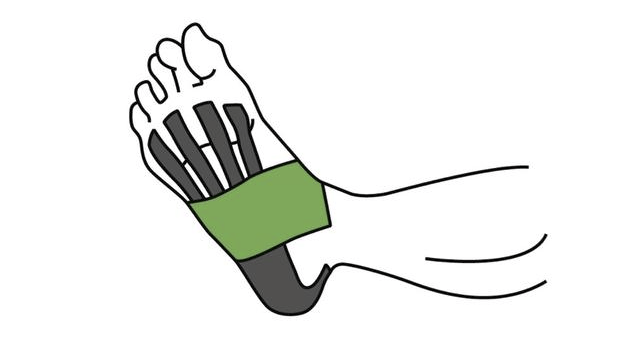
• Taping: temporary of support for the strained plantar fascia can be provided with figure-eight taping or with low-dye strapping
• Restricted activity: repetitive and straining activities should be strictly limited, intiaially. Immobilization is not recommended.
• Cryotherapy: Ice massage and/or cold packs help reduce pain and inflammation.
Healing
• Ultrasound: Initially pulsed, then constant and direct (once inflammation has subsided).
• Transverse friction massage: to stimulate blood flow and collagen deposition.3
• Vitamin C with bioflavonoids: a natural anti-inflammatory that can speed healing
Adjustments
• Calcaneus: Reduction of the calcaneus posteririty to relieve sagittal stress. Kell’s technique uses a posterior-to-anterior thrust on a table with a pelvic drop piece.4
• Other foot joints: Brantingham found various areas of joint dysfunction in the tarsal and metatarsal koints in patients with plantar fasciitis.5 The navicular and first metatarsophalangeal joints are often involved.
Orthotic Support
• Orthotics for pronation: to support the arches and reduce the stress on the plantar fascia
• Orthotics for supination: arch support with added visco-elastic material to cushion the foot and decrease the amounf of shock at heel strike.
• Heel spur correction: A “divot†in the surface of the material under the heel to spread pressure away from the fascial insertion.
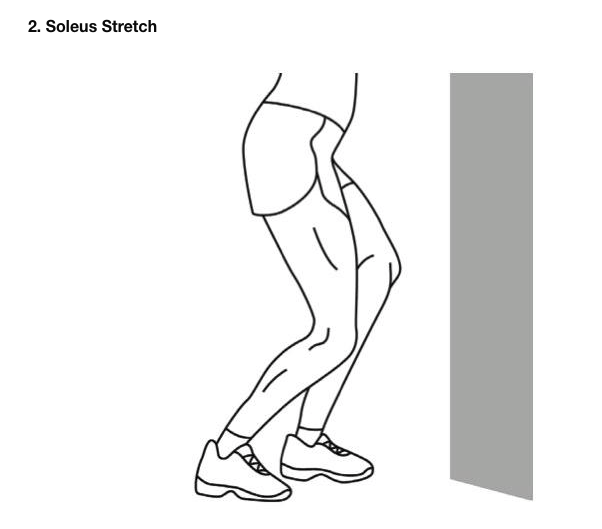
Heel and foot stretching: “Runner’s stretch†for the calf and the bottom of the foot.
• Intrinsic muscle strengthening: Toe curl excercises (while sitting, gather a towel on the floor up under the arch, and repeat three times).
• Extrinsic muscle strengthening: Toe raises (while standing on the edge of a stai, slowly rise up on balls of feet) and ankle stabilizing series with tubing
Conclusion
Plantar fasciitis usually responds well to focused, conservative treatment. Steroid injections and surgical release are seldom necessary and are best avoided. One of the most important treatment methods is to reduce any tendency to pronate excessively. In addition to custom-fitted orthotics, runner should wear well-designed shoes that provide good heel stability. The use of corrective orthotics can prevent many overuse problems from developing in the lower extremeties. Investigation of foot biomechanics is a good idea for all patients but especially those who are recreationally active.
This blog was curated from the article titled “Plantar Fasciitis†by John K. Hyland, DC, DACBR, DABCO, CSCS and was published in the magazing The American Chiropractor Volume 38.
References:
1. Â Â Â Lapidus PW, Guidotti FP. Painful heel: report of 323 patients with 364 painful heels. Clun Orthop 1965;39;178.
2. Â Â Â Subotnick SI. Sports medicine of the lower extremity. New York; Churchill Livingston; 1989:237.
3. Â Â Â Lear L. Transverse friction massage. Sports Med Update 1996;10:18-25.
4. Â Â Â Kell PM. A comparative radiologic examination for unresponsive plantar fasciitis. J Manip Physiol Therap 1994;17:329-34.
5. Â Â Â Kibler WB, et al. Functional rehabilitation of sports and musculoskeletal injuries. Gaithersburg, MA: Aspen Publishers; 1998:280.
Post Disclaimer
Professional Scope of Practice *
The information herein on "Treating Plantar Fasciitis" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness, Personal Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those on this site and our family practice-based chiromed.com site, and focuses on restoring health naturally for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
Licenses and Board Certifications:
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card








 Again, We Welcome You.
Again, We Welcome You.
Comments are closed.