Herniated lumbar discs, although considered common, can be very debilitating and disabling. While it may be impossible to prevent disc herniations, understanding the mechanism of injury and implementing that knowledge can cut the odds of developing this unpleasant injury. A range of factors may promote lumbar disc damage or injury. The mechanism of injury for herniated discs often involves flexion, compression and twisting of the lumbar spine.
Table of Contents
Mechanism of Injury: Herniated Discs
The lumbar spine’s discs are specialized connective tissue structures which function as shock absorbers between the spinal bones or vertebrae of the spine. Intervertebral discs are springy in nature due to a moist, jelly-like center portion known as the nucleus pulposus. The nucleus pulposus is contained and surrounded by a more layered, fibrous tissue that makes up what is known as the annulus fibrosis. Herniated discs or ruptured discs occur when harm to the annulus fibrosis causes the nucleus pulposus material to escape its boundaries and protrude outward in the disc.
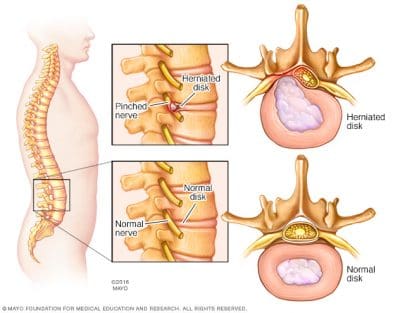
Flexion
Where lumbar disc herniations occur regularly in a normal setting, these aren’t easily reproduced in a research setting. It is notable that in scientific research studies, where disc herniations were created in animal or human lumbar spine specimens, most demanded a small amount of spine flexion. Because of this, Stuart McGill, Ph.D., author of the book “Low Back Disorders,” concludes that repeated or prolonged spine flexion will be the primary mechanism leading to lumbar disc herniation. In a lab setting, McGill and other scientific doctors found that the way they could produce herniated disc injuries was to place weight, or a weight, onto the spine while bending into flexion. These circumstances are consistent with what could happen with repetitive lifting activities where the spine is flexed forward.
Compression
A research presented in 2001 in the journal “Clinical Biomechanics” demonstrated a link between compression of the spinal joints, technically known as vertical loading, and disc herniation. Even though the analysis used spinal sections taken from the necks of pigs, the researchers tried to replicate loading patterns common to the lumbar spines of humans. In the scientific study, severe and more frequent cases of herniated discs resulted when compression forces on the spinal bones had been increased. However, compression forces were essential to cause damage or injury such as disc herniations, that were subjected to repetitions of forward and backward bending. The authors reasoned that flexion and extension moves likely play a larger part than compression alone in inducing disc herniations. To put it differently, the spine can resist compression forces, such as lifting, when in a vertical position. Including a load whilst bending forward and backward though, may quickly spell difficulty for the individual.
Twisting
Another study published in 2010 in “Cinical Biomechanics” analyzed the role of axial torque, or twisting, in disc herniation. Using an animal model, the researchers discovered that disc herniation was not caused by twisting that was isolated. However, twisting did damage the annulus fibrosis. With damage to the annulus, the discs were more vulnerable to rupture or herniation when subjected to flexion movements. This implies that if the mechanism of injury of a disc herniation is flexion, these may be contributed to by damage brought on by twisting weakened discs.
Occupational Factors
A study published in 1987 in the “Journal of Chronic Diseases” examined the risk of lumbar herniated discs associated with occupation. The researchers noted that the risk for this condition is greater among men in blue-collar jobs in contrast to those in white collar jobs. This relates to increased lifting and bending activities among blue-collar workers when compared with white-collar employees. The writers noted less variation by occupational groups among women. The risk of lumbar disc herniations, however, was greater among women who described their work as strenuous. An additional finding that may relate to the spinal flexion mechanism of injury is that the risk of lumbar disc herniations is high among individuals whose work entails driving an automobile. Sitting while driving places the lumbar spine in a sustained posture of slight flexion.
Diagnosis for Herniated Discs
Lower back pain and symptoms associated with sciatica, are common manifestations resulting from lumbar spine disc herniation. Healthcare professionals, including chiropractors who specialize in sciatica, can help diagnose herniated discs as well as help determine the source of the individual’s symptoms. A spine specialist may provide the patient with or direct them to a clinic to have x-rays, MRI’s or CT scans to properly determine the presence of a herniated disc. Seeking immediate medical attention is essential towards the patient’s recovery.
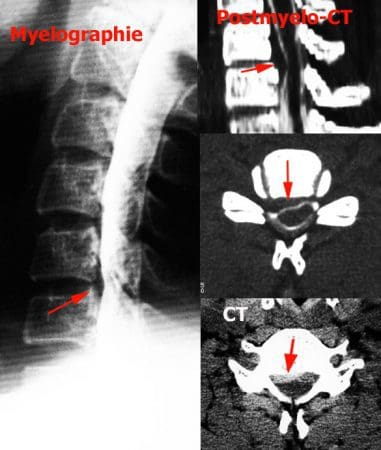
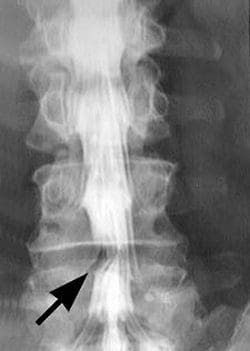
MRI of a Lumbar Herniated Disc
The scope of our information is limited to chiropractic and spinal injuries and conditions. To discuss options on the subject matter, please feel free to ask Dr. Jimenez or contact us at 915-850-0900 . 
By Dr. Alex Jimenez
Additional Topics: Sciatica
Lower back pain is one of the most commonly reported symptoms among the general population. Sciatica, is well-known group of symptoms, including lower back pain, numbness and tingling sensations, which often describe the source of an individual’s lumbar spine issues. Sciatica can be due to a variety of injuries and/or conditions, such as spinal misalignment, or subluxation, disc herniation and even spinal degeneration.

TRENDING TOPIC: EXTRA EXTRA: New PUSH 24/7Â®ï¸ Fitness Center
Post Disclaimer
Professional Scope of Practice *
The information herein on "Scientific Chiropractor: Causes Of Lumbar Herniated Discs" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness, Personal Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those on this site and our family practice-based chiromed.com site, and focuses on restoring health naturally for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
Licenses and Board Certifications:
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card




 Again, We Welcome You.
Again, We Welcome You.
Comments are closed.