Non-radiographic axial spondyloarthritis or nr-axSpA and non-radiographic ankylosing spondylitis/AS are related. However, non-radiographic axial spondyloarthritis can present AS symptoms with active inflammation of the spine and sacroiliac/SI joints, causing back and hip pain but does not reveal joint damage on X-rays or MRIs. Injury Medical Chiropractic and Functional Medicine Clinic can explain what it means to have non-radiographic axial spondyloarthritis, how it can be managed, and what to do to prevent it from turning into ankylosing spondylitis.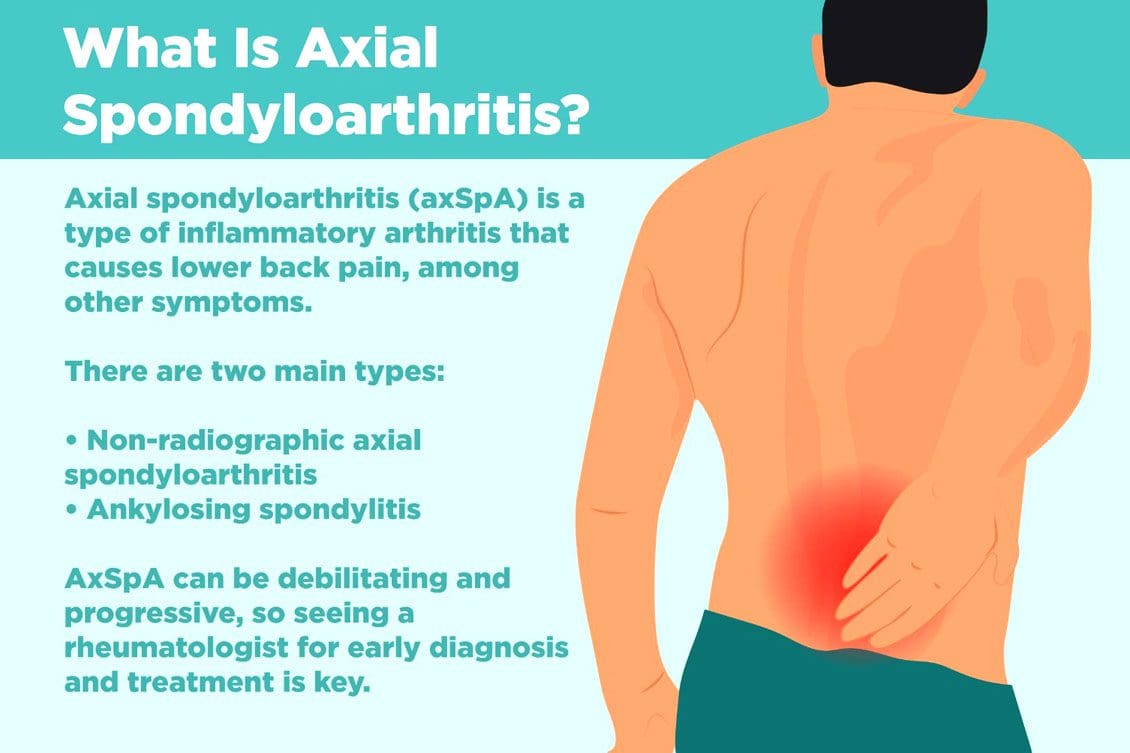
Table of Contents
Non-Radiographic Axial Spondyloarthritis
Non-radiographic axial spondyloarthritis means there are early AS symptoms but have not developed enough joint inflammation or damage to show up on an X-ray or other form of imaging. Early evidence of joint inflammation includes blurring of the joint edges and localized regions of joint erosion. It can be difficult for physicians to see these subtle changes on an x-ray.
Ankylosing Spondylitis
- Ankylosing spondylitis, or AS, is a form of inflammatory arthritis that affects joints in the spine and elsewhere.
- It is a chronic, inflammatory, autoimmune disease.
- Medical research is still ongoing to determine the exact cause, but a genetic component is believed to be contributing factor.
- Around 85% of individuals with ankylosing spondylitis have inherited the HLA-B27 gene, which is associated with multiple autoimmune conditions.
- In the early stages, individuals will present lower back pain around the sacroiliac joints or the joints that connect the spine to the pelvis.
- Later stages have more obvious X-ray findings, like the fusing of the sacroiliac joints and the lower spine that takes place over time.
- Joint inflammation can progress, causing permanent joint damage and spine rigidity.
- Most individuals with the condition can manage their symptoms with NSAIDs, chiropractic care, physical and massage therapy, and range of motion exercises.
Stage 1
- There is no evidence of spinal inflammation on x-rays.
- MRI provides more detailed images of bones and may reveal bone marrow edema or accumulation of fluid in the structures of the spinal bones and joints.
- Individuals with non-radiographic axial spondyloarthritis, you are here.
Stage 2
- There is visible inflammation of the spinal joints on the x-ray.
- The sacroiliac joints between the spine and the pelvis are the most affected.
Stage 3
- Chronic inflammation of the joints has caused bone loss and permanent joint damage, resulting in spine rigidity.
Symptoms of Non-Radiographic Axial Spondyloarthritis
There are differences between back pain associated with muscle strain and arthritis. Back pain symptoms include:
- Starts to present before age 40.
- It has a gradual onset and can go unnoticed for years.
- Improves with movement or activity.
- Eases up throughout the day.
- Starts up in the evening when resting.
Other symptoms include:
- Joint stiffness
- Swollen fingers
- Heel pain
- Bilateral buttock discomfort and pain
Slowing Progression
Progression from non-radiographic axial spondyloarthritis to ankylosing spondylitis occurs in 10% – 20% of individuals over a two-year period. Progression factors include genetics, gender, degree of joint damage, and level of inflammatory markers at the time of diagnosis.
- Early diagnosis and treatment can slow the progression before significant joint damage with anti-inflammatory therapy, rheumatological therapy, and targeted exercise.
- Work with a specialist like an orthopedic spine specialist and rheumatologist that understands the disorder and is up to date on the most recent treatment modalities.
- A rheumatologist will perform diagnostic tests, including spine X-rays, genetic blood work, and serum inflammatory markers.
- Individuals with non-radiographic axial spondyloarthritis should expect to have serial X-rays to gauge the progression of the disease.
- Staying healthy and active is recommended to slow the progression of nr-AxSpA and AS.
- Recent medical advances and lifestyle adjustments can slow the progression in most cases.
axSpA
References
Six tips for living well with ankylosing spondylitis. Available at https://www.mayoclinic.org/diseases-conditions/ankylosing-spondylitis/in-depth/6-tips-for-living-well-with-ankylosing-spondylitis/art-20478753. Accessed 11/07/2022.
Ankylosing spondylitis. Mayo Clinic. Available at https://www.mayoclinic.org/diseases-conditions/ankylosing-spondylitis/symptoms-causes/syc-20354808. Accessed 11/05/2022.
D. J. Pradeep, A. Keat, K. Gaffney, Predicting outcome in ankylosing spondylitis, Rheumatology, Volume 47, Issue 7, July 2008, Pages 942–945, https://doi.org/10.1093/rheumatology/ken195
Kucyba?a, Iwona, et al. “Radiologic approach to axial spondyloarthritis: where are we now and where are we heading?.” Rheumatology international vol. 38,10 (2018): 1753-1762. doi:10.1007/s00296-018-4130-1
Michelena, Xabier, López-Medina, Clementina, and Helena Marzo-Ortega. “Non-radiographic versus radiographic axSpA: what’s in a name?”.” National Center for Biotechnology Information. October 14, 2020. https://doi.org/10.1093/rheumatology/keaa422
Swift D. Ankylosing spondylitis: disease progression varies widely. Medpage Today. Accessed 11/05/2022.Available at https://www.medpagetoday.com/rheumatology/arthritis/49096
Post Disclaimer
Professional Scope of Practice *
The information herein on "Non-Radiographic Axial Spondyloarthritis: Chiropractic Scientists" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness, Personal Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those on this site and our family practice-based chiromed.com site, and focuses on restoring health naturally for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
Licenses and Board Certifications:
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card





 Again, We Welcome You.
Again, We Welcome You.
Comments are closed.