El Paso,TX. Chiropractor Dr. Alex Jimenez looks examines a herniated disc.
Herniated disc is a somewhat common condition that can occur anywhere along the spinal column, but most commonly affects the lower back or neck area. Also known as ruptured disk or a slipped disc, a herniated disc develops when one of the pillow-like pads between the vertebrae moves out of position and presses on nerves that are adjacent.
Herniated discs are usually caused by overuse injuries or injury to the back; however, disc conditions may also develop as a result of the standard aging process. It’s also known that there is a genetic factor that leads to the evolution of herniated disc and disc degeneration. As the size of herniation shrinks with time via resorption, typically, a herniated disc in the lower back will heal within six months. If physical therapy, drugs along with other treatments fail, operation may be needed.
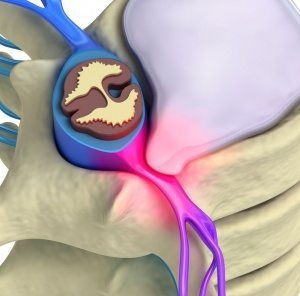
Table of Contents
What’s A Disc?
Spinal discs are cushion-like pads located between the vertebrae. Without these “shock absorbers,†the bones in the spinal column would grind against one another. Along with giving the backbone flexibility and making movements like twisting and bending potential, discs protect the spine by absorbing the effect of trauma and body weight. Each disk has a strong outer layer called annulus fibrosus and a soft, gel-like center, called nucleus pulposus. There are fibers on the outside of each disc that attach to adjoining vertebrae and hold the disc in position. A herniated disc occurs when the gel as well as the outer layer tears or ruptures -like middle leaks to the spinal canal.
The spinal canal has only enough space to place spinal fluid and the spinal cord. When a disc herniates and spills to the spinal canal, it could cause compression of spinal cord or the nerves. Alterations in sensation and intense, debilitating pain often happen. Furthermore, the gel-like substance inside the disk releases chemical irritants that bring about pain and nerve inflammation.
What Causes A Herniated Disc?
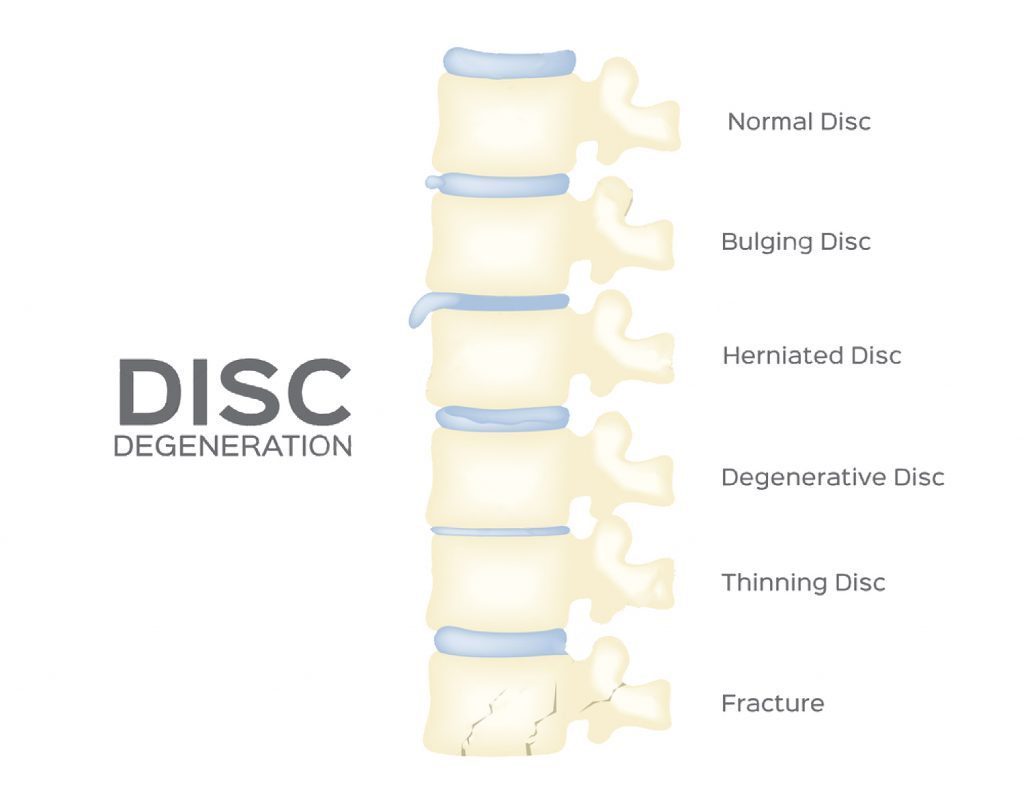
As we get older, the spinal disks gradually lose fluid volume. This process progresses slowly and begins at about age 30, over time. As the disks dry out, tears or microscopic cracks can form on the outer surface, causing it to become weak, fragile and much more susceptible to injury. The most common causes of herniated disc are:
- Wear and tear: Disks dry out and aren’t as adaptive as they were.
- Repetitive movements: Work, lifestyle, and certain sports activities that place stress on the spine, especially the lower back, further weaken an already vulnerable area.
- Lifting the wrong way: Never lift while bent at the waist. Proper lifting entails lifting with a straight back and your legs.
- Injury: High-impact trauma can create the disk to bulge, tear or rupture.
- Obesity: Carrying excess weight places an undue amount of strain on the back.
- Genetics: There are a few genes which might be more typically present in individuals with disc degeneration. More research is necessary to investigate the role of those genes—they could be targets of biological treatment in the future.
Which Are The Symptoms Of A Herniated Disc?
Pain from a herniated disc can fluctuate, determined by severity and the place of the harm. It is typically felt on one side of the body.
Little or no pain could be felt in case the injury is minimal. Pain might be severe and unrelenting, in the event the disk ruptures. If significant nerve impingement has occurred pain may radiate to an extremity in a certain nerve root distribution. For instance, sciatica is often resulting from herniated disc in the low back. Herniated disc can manifest itself with a variety of symptoms, including:
- Dull ache to severe pain
- Numbness, tingling, burning
- Muscle weakness; spasm; altered reflexes
- Loss in bowel or bladder control (Note: These symptoms constitute a medical emergency. When they occur, seek medical attention immediately).
How Is A Herniated Disc Diagnosed?
History and physical examination point to some diagnosis of herniated disc. A herniated disc is likely if low back pain is accompanied by radiating leg pain in a nerve root distribution with positive straight leg raising test (ie, elevating the leg while lying down causes radiating pain down the leg), as well as other neurologic deficits for example numbness, weakness, and altered reflexes.
Imaging studies usually are ordered to confirm a diagnosis of herniated disc. X rays are not the imaging medium of choice because soft tissues (eg, discs, nerves) are hard to capture with this specific technology. However, they might be used as an initial tool to eliminate other illnesses such as for instance fracture or a growing. Confirmation of the feeling of herniated disc is generally achieved with:
- Magnetic Resonance Imaging (MRI): This technology shows the spinal cord, surrounding soft tissue and nerves. It really is the best imaging study to support the identification of a herniated disc.
- Nerve Conduction Studies (NCS) and Electromyogram (EMG): These studies use electric impulses to measure the level of harm to the nerve/s brought on by compaction from a herniated disc along with other conditions that cause nerve impingement may be ruled out. NCS and EMG are not routine evaluations to diagnose herniated disc.
Herniated discs occasionally heal independently through a process called resorption. This means the disk fragments are consumed by the body. Most people suffering from herniated disc do not need surgery and react well to conservative treatment.
Post Disclaimer
Professional Scope of Practice *
The information herein on "Herniated Disc Center" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness, Personal Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those on this site and our family practice-based chiromed.com site, and focuses on restoring health naturally for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
Licenses and Board Certifications:
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card





 Again, We Welcome You.
Again, We Welcome You.
Comments are closed.