El Paso, Tx. Wellness chiropractor, Dr. Alexander Jimenez examines Functional Medicine. What it is and how it can help in having a healthy lifestyle.
Table of Contents
The Challenge
Of total healthcare costs in the United States, more than 86% is due to chronic conditions.1 In 2015, health care spending reached $3.2 trillion, accounting for 17.8% of GDP.2 This exceeded the combined federal expenditures for national defense, homeland security, education, and welfare. By 2023, if we don’t change how we confront this challenge, annual healthcare costs in the U.S. will rise to over $4 trillion,3,4 the equivalent—in a single year—of four Iraq wars, making the cost of care using the current model economically unsustainable. If our health outcomes were commensurate with such costs, we might decide they were worth it. Unfortunately, the U.S. spends twice the median per-capita costs of other industrialized countries, as calculated by the Organization for Economic Cooperation and Development (OECD),5 despite having relatively poor outcomes for such a massive investment.6
Our current healthcare model fails to confront both the causes of and solutions for chronic disease and must be replaced with a model of comprehensive care geared to effectively treating and reversing this escalating crisis.This transformation requires something different than is usually available in our very expensive healthcare system.7
A Contributing Factor—Outdated Clinical Model
Despite notable advances in treating and preventing infectious disease and trauma, the acute-care model that dominated 20th century medicine has not been effective in treating and preventing chronic disease.
 Adopting a new operating system for 21st century medicine requires that we:
Adopting a new operating system for 21st century medicine requires that we:
- Recognize and validate more appropriate and successful clinical models
- Re-shape the education and clinical practices of health professionals to help them achieve proficiency in the assessment, treatment, and prevention of chronic disease
- Reimburse equitably for lifestyle medicine and expanded preventive strategies, acknowledging that the greatest health threats now arise from how we live, work, eat, play, and move
 This problem can’t be solved by drugs and surgery, however helpful those tools may be in managing acute signs and symptoms. It can’t be solved be adding new or unconventional tools, such as botanical medicine and acupuncture, to a failing model. It can’t be solved by pharmacogenomics (although advances in that discipline should help reduce deaths from inappropriately prescribed medication—estimated to be the fourth leading cause of hospital deaths12). The costly riddle of chronic disease can only be solved by shifting our focus from suppression and management of symptoms to addressing their underlying causes. Specifically, we must integrate what we know about how the human body works with individualized, patient-centered, science-based care that addresses the causes of complex, chronic disease, which are rooted in lifestyle choices, environmental exposures, and genetic influences.
This problem can’t be solved by drugs and surgery, however helpful those tools may be in managing acute signs and symptoms. It can’t be solved be adding new or unconventional tools, such as botanical medicine and acupuncture, to a failing model. It can’t be solved by pharmacogenomics (although advances in that discipline should help reduce deaths from inappropriately prescribed medication—estimated to be the fourth leading cause of hospital deaths12). The costly riddle of chronic disease can only be solved by shifting our focus from suppression and management of symptoms to addressing their underlying causes. Specifically, we must integrate what we know about how the human body works with individualized, patient-centered, science-based care that addresses the causes of complex, chronic disease, which are rooted in lifestyle choices, environmental exposures, and genetic influences.
This perspective is completely congruent with what we might call the “omics†revolution. Formerly, scientists believed that once we deciphered the human genome we would be able to answer almost all the questions about the origins of disease.What we actually learned, however, is that human biology is far more complex than that. In fact, humans are not genetically hardwired for most diseases; instead, gene expression is altered by myriad influences, including environment, lifestyle, diet, activity patterns, psycho-social-spiritual factors, and stress.These lifestyle choices and environmental exposures can push us toward (or away from) disease by turning on—or o — certain genes.That insight has helped to fuel the global interest in Functional Medicine, which has that principle at its very core.
A Strategic Response
Functional Medicine directly addresses the underlying causes of disease by using a systems-oriented approach with transformative clinical concepts, original tools, an advanced process of care (see box below), and by engaging both patient and practitioner in a therapeutic partnership.

Functional Medicine practitioners look closely at the myriad interactions among genetic, environmental, and lifestyle factors that can influence long-term health and complex, chronic disease (see Figure 1).A major premise of Functional Medicine is that, with science, clinical wisdom, and innovative tools, we can identify many of the underlying causes of chronic disease and intervene to remediate the clinical imbalances, even before overt disease is present.
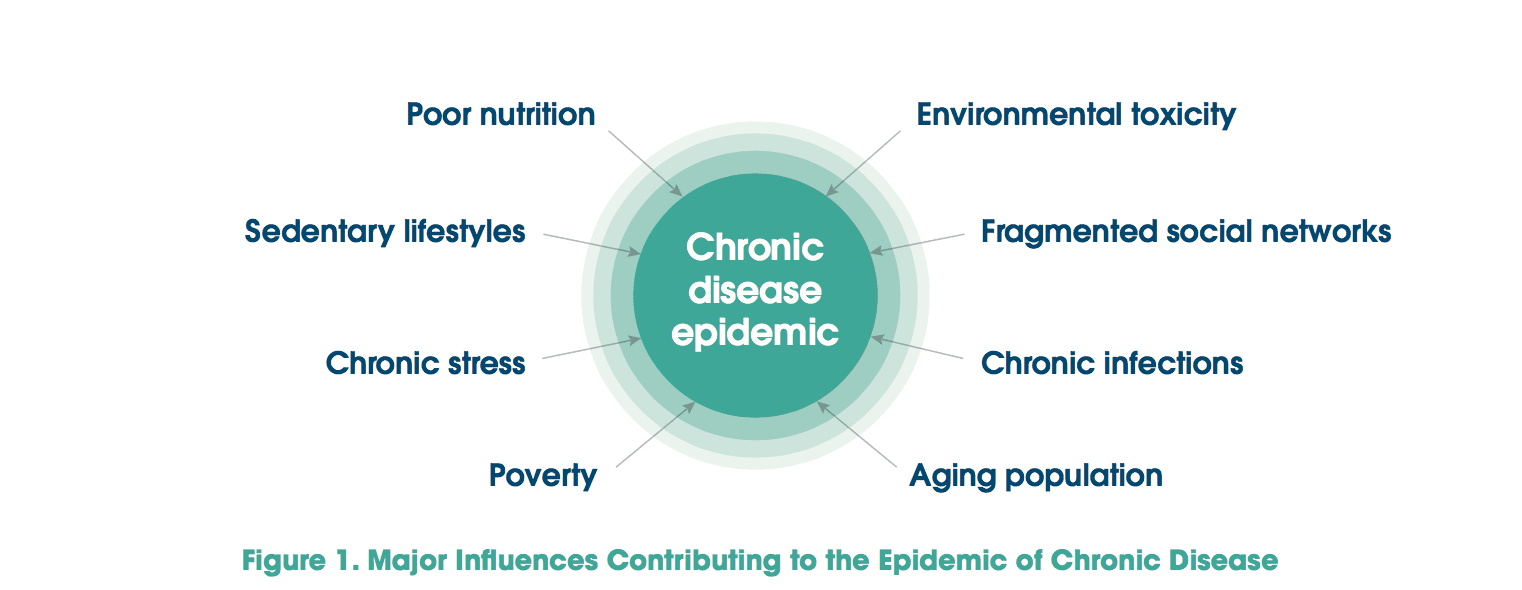
Functional Medicine exemplifies just the kind of systems-oriented, personalized medicine that is needed to transform clinical practice.The Functional Medicine model of comprehensive care and primary prevention for complex, chronic illness is grounded in both science (evidence about common underlying mechanisms and pathways of disease as well as evidence about the contributions of environmental and lifestyle factors to disease) and art (the healing partnership and the search for insight in the therapeutic encounter).
What Is Functional Medicine?
Functional Medicine asks how and why illness occurs and restores health by addressing the root causes of disease for each individual. It is an approach to health care that conceptualizes health and illness as part of a continuum in which all components of the human biological system interact dynamically with the environment, producing patterns and effects that change over time. Functional Medicine helps clinicians identify and ameliorate dysfunctions in the physiology and biochemistry of the human body as a primary method of improving patient health. Chronic disease is almost always preceded by a period of declining function in one or more of the body’s systems. Functional Medicine is often described as the clinical application of systems biology. Restoring health requires reversing (or substantially improving) the specific dysfunctions that have contributed to the disease state. Each patient represents a unique, complex, and interwoven set of environmental and lifestyle influences on intrinsic functionality (their genetic vulnerabilities) that have set the stage for the development of disease or the maintenance of health.
To manage the complexity inherent in this approach, IFM has created practical models for obtaining and evaluating clinical information that lead to individualized, patient-centered, science-based therapies. Functional Medicine concepts, practices, and tools have evolved considerably over a 30-year period, reflecting the dramatic growth in the evidence base concerning the key common pathways to disease (e.g., inflammation, oxidative stress); the role of diet, stress, and physical activity; the emerging sciences of genomics, proteomics, and metabolomics; and the effects of environmental toxins (in the air, water, soil, etc.) on health.
Elements Of Functional Medicine
The knowledge base—or “footprintâ€â€”of Functional Medicine is shaped by six core foundations:
- Gene-Environment Interaction: Functional Medicine is based on understanding the metabolic processes of each individual at the cellular level. By knowing how each person’s genes and environment interact to create their unique biochemical phenotype, it is possible to design targeted interventions that correct the specific issues that lead to destructive processes such as inflammation and oxidation, which are at the root of many diseases.
- Upstream Signal Modulation: Functional Medicine interventions seek to influence biochemical pathways “upstream†and prevent the overproduction of damaging end products, rather than blocking the effects of those end products. For example, instead of using drugs that block the last step in the production of inflammatory mediators (NSAIDs, etc.), Functional Medicine treatments seek to prevent the upregulation of those mediators in the first place.
- Multimodal Treatment Plans: The Functional Medicine approach uses a broad range of interventions to achieve optimal health including diet, nutrition, exercise and movement; stress management; sleep and rest, phytonutrient, nutritional and pharmaceutical supplementation; and various other restorative and reparative therapies.These interventions are all tailored to address the antecedents, triggers, and mediators of disease or dysfunction in each individual patient.
- Understanding the Patient in Context: Functional Medicine uses a structured process to uncover the significant life events of each patient’s history to gain a better understanding of who they are as an individual. IFM tools (the “Timeline†and the “Matrix†model) are integral to this process for the role they play in organizing clinical data and mediating clinical insights.This approach to the clinical encounter ensures that the patient is heard, engenders the therapeutic relationship, expands therapeutic options, and improves the collaboration between patient and clinician.
- Systems Biology-Based Approach: Functional Medicine uses systems biology to understand and identify how core imbalances in specific biological systems can manifest in other parts of the body. Rather than an organ systems-based approach, Functional Medicine addresses core physiological processes that cross anatomical boundaries including: assimilation of nutrients, cellular defense and repair, structural integrity, cellular communication and transport mechanisms, energy production, and biotransformation.The “Functional Medicine Matrix†is the clinician’s key tool for understanding these network effects and provides the basis for the design of effective multimodal treatment strategies.
- Patient-Centered and Directed: Functional Medicine practitioners work with the patient to find the most appropriate and acceptable treatment plan to correct, balance, and optimize the fundamental underlying issues in the realms of mind, body, and spirit. Beginning with a detailed and personalized history, the patient is welcomed into the process of exploring their story and the potential causes of their health issues. Patients and providers work together to determine the diagnostic process, set achievable health goals, and design an appropriate therapeutic approach.
To assist clinicians in understanding and applying Functional Medicine, IFM has created a highly innovative way of representing the patient’s signs, symptoms, and common pathways of disease. Adapting, organizing, and integrating into the Functional Medicine Matrix the seven biological systems in which core clinical imbalances are found actually creates an intellectual bridge between the rich basic science literature concerning physiological mechanisms of disease and the clinical studies, clinical diagnoses, and clinical experience acquired during medical training.These core clinical imbalances serve to marry the mechanisms of disease with the manifestations and diagnoses of disease.
- Assimilation: digestion, absorption, microbiota/GI, respiration
- Defense and repair: immune, inflammation, infection/microbiota
- Energy: energy regulation, mitochondrial function
- Biotransformation and elimination: toxicity, detoxification
- Transport: cardiovascular and lymphatic systems
- Communication: endocrine, neurotransmitters, immune messengers
- Structural integrity: sub-cellular membranes to musculoskeletal integrity
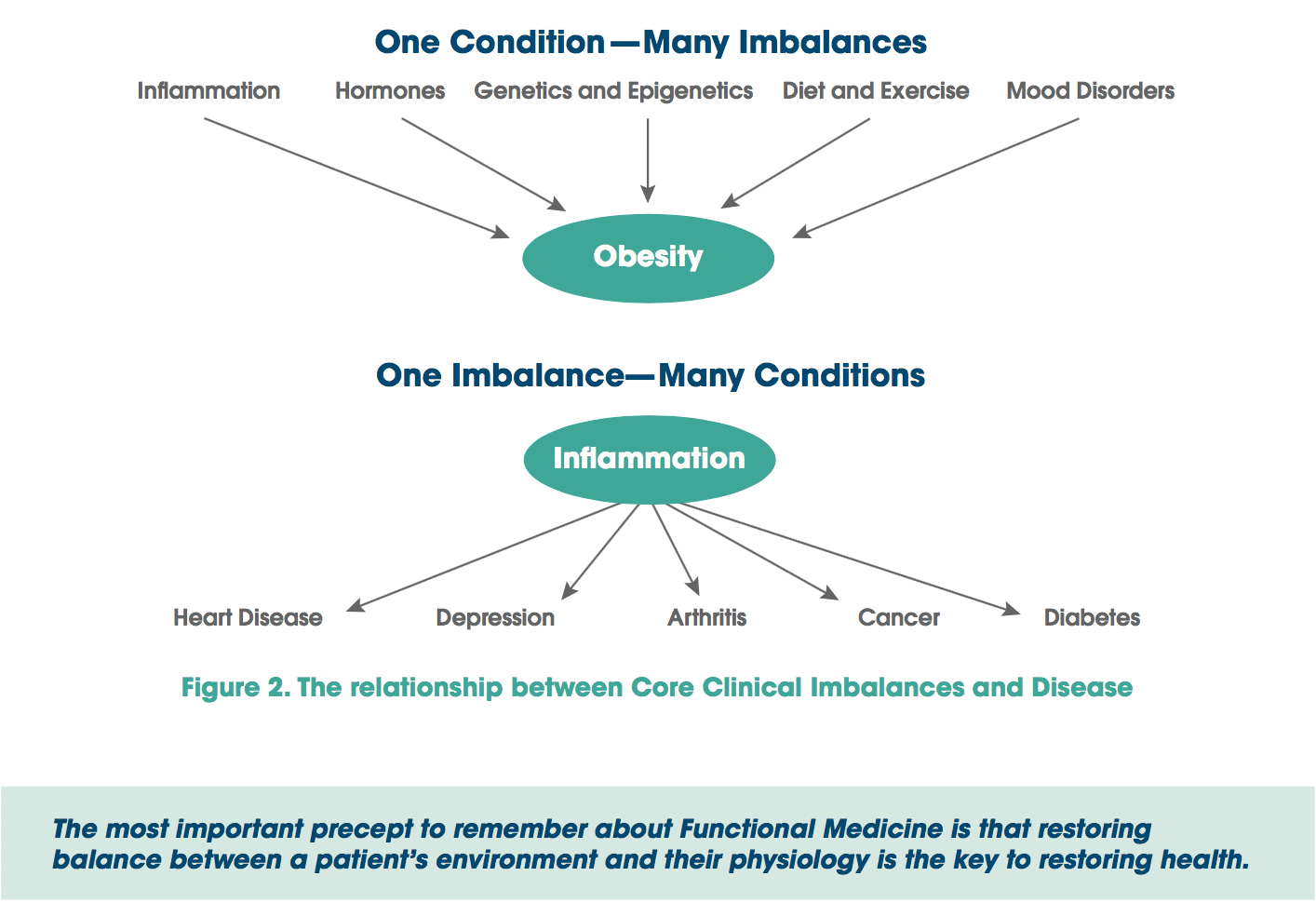
Using this construct, it is possible to see that one disease/condition may have multiple causes (i.e., multiple clinical imbalances), just as one fundamental imbalance may be at the root of many seemingly disparate conditions (see Figure 2).
 Constructing The Model & Putting It Into Practice
Constructing The Model & Putting It Into Practice
The scientific community has made incredible strides in helping practitioners understand how environment and lifestyle, interacting continuously through an individual’s genetic heritage, psychosocial experiences, and personal beliefs, can impair one or all of the seven core clinical imbalances. IFM has developed concepts and tools that help to collect, organize, and make sense of the data gathered from an expanded history, physical exam, and laboratory evaluation, including:
The GOTOIT system, which presents a logical method for eliciting the patient’s whole story and ensuring that assessment and treatment are in accord with that story:
G = Gather Information
O = Organization Information
T = Tell the Complete Story Back to the Patient
O = Order and Prioritize
I = InitiateTreatment
T = Track Outcomes
- The Functional Medicine Timeline, which helps to connect key events in the patient’s life with the onset of symptoms of dysfunction.
- The Functional Medicine Matrix, which provides a unique and succinct way to organize and analyze all of a patient’s health data (see Figure 3).
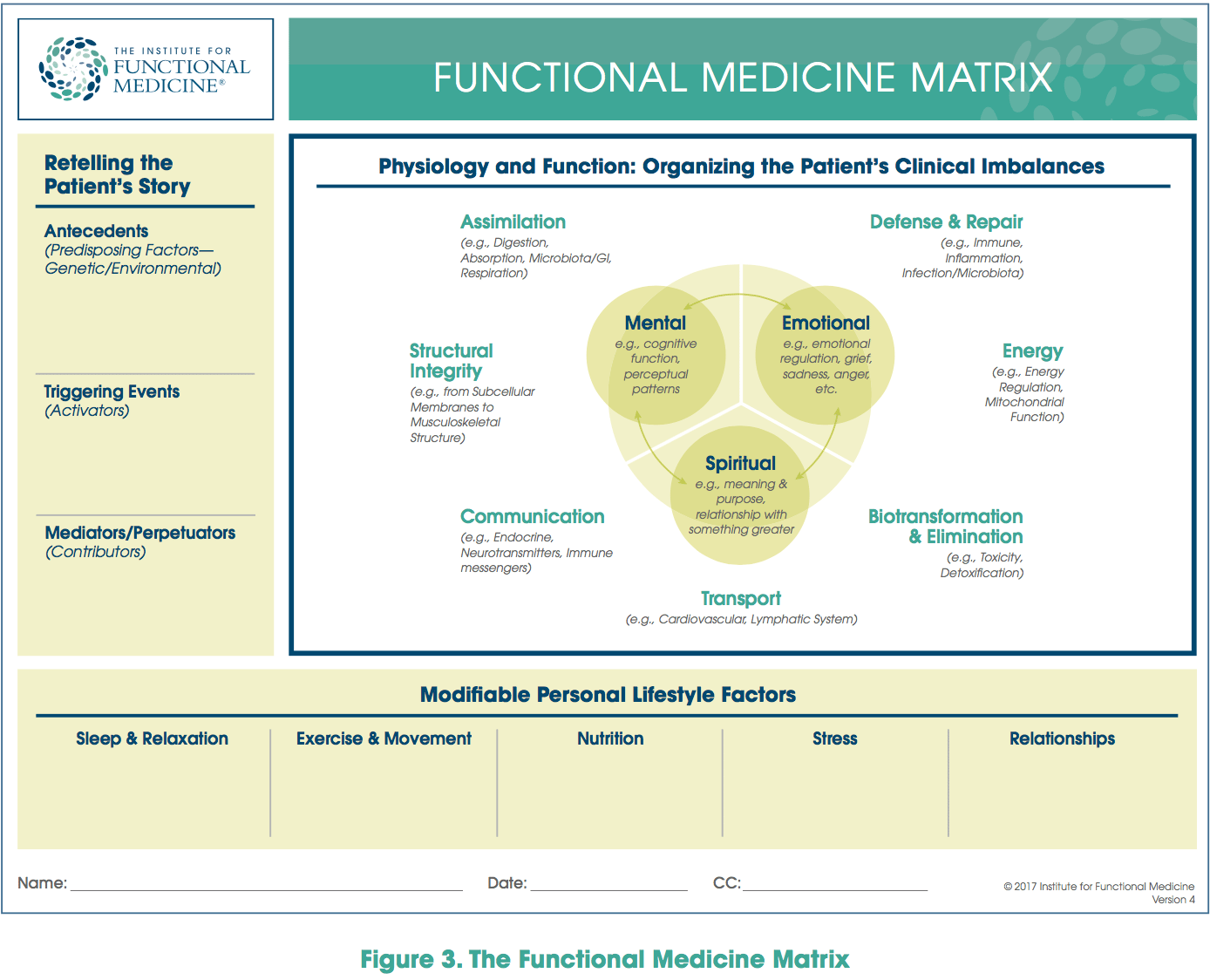 The patient’s lifestyle influences are entered across the bottom of the Matrix, and the Antecedents,Triggers, and Mediators (ATMs) of disease/dysfunction are entered in the upper left corner.The centrality of the patient’s mind, spirit, and emotions, with which all other elements interact, is clearly shown in the figure. Using this information architecture, the clinician can create a comprehensive snapshot of the patient’s story and visualize the most important clinical elements of Functional Medicine:
The patient’s lifestyle influences are entered across the bottom of the Matrix, and the Antecedents,Triggers, and Mediators (ATMs) of disease/dysfunction are entered in the upper left corner.The centrality of the patient’s mind, spirit, and emotions, with which all other elements interact, is clearly shown in the figure. Using this information architecture, the clinician can create a comprehensive snapshot of the patient’s story and visualize the most important clinical elements of Functional Medicine:
1. Identifying each patient’s ATMs of disease and dysfunction.
2. Discovering the factors in the patient’s lifestyle and environment that influence the expression of health or disease.
3. Applying all the data collected about a patient to a matrix of biological systems, within which disturbances in function originate and are expressed.
4. Integrating all this information to create a comprehensive picture of what is causing the patient’s problems, where they are originating, what has influenced their development, and—as a result of this critical analysis—where to intervene to begin reversing the disease process or substantially improving health.
A Functional Medicine treatment plan may involve one or more of a broad range of therapies, including many different dietary interventions (e.g., elimination diet, high phytonutrient diversity diet, low glycemic-load diet), nutraceuticals (e.g., vitamins, minerals, essential fatty acids, botanicals), and lifestyle changes (e.g., improving sleep quality/quantity, increasing physical activity, decreasing stress and learning stress management techniques, quitting smoking). Nutrition is so vital to the practice of Functional Medicine that IFM has established a core emphasis on Functional Nutrition and has funded the development of a set of unique, innovative tools for developing and applying dietary recommendations.
Scientific support for the Functional Medicine approach to treatment can be found in a large and rapidly expanding evidence base about the therapeutic effects of nutrition (including both dietary choices and the clinical use of vitamins, minerals, and other nutrients such as sh oils)13,15,15; botanicals16,17,18; exercise19 (aerobics, strength training, flexibility); stress management 20; detoxification 21,22,23; acupuncture 24,25,26; manual medicine (massage, manipulation)27,28,29; and mind/body techniques 30,31,32 such as meditation, guided imagery, and biofeedback.
All of this work is done within the context of an equal partnership between the practitioner and patient.The practitioner engages the patient in a collaborative relationship, respecting the patient’s role and knowledge of self, and ensuring that the patient learns to take responsibility for their own choices and for complying with the recommended interventions. Learning to assess a patient’s readiness to change and then providing the necessary guidance, training, and support are just as important as ordering the right lab tests and prescribing the right therapies.
Summary
The practice of Functional Medicine involves four essential components: (1) eliciting the patient’s complete story during the Functional Medicine intake; (2) identifying and addressing the challenges of the patient’s modifiable lifestyle factors and environmental exposures; (3) organizing the patient’s clinical imbalances by underlying causes of disease in a systems biology matrix framework; and (4) establishing a mutually empowering partnership between practitioner and patient.
A great strength of Functional Medicine is its relevance to all healthcare disciplines and medical specialties, any of which can—to the degree allowed by their training and licensure—apply a Functional Medicine approach, using the Matrix as a basic template for organizing and coupling knowledge and data. In addition to providing a more effective approach to preventing, treating, and reversing complex chronic disease, Functional Medicine can also provide a common language and a uni ed model that can be applied across a wide variety of health professions to facilitate integrated care.
Functional Medicine is playing a key role in the effort to solve the modern epidemic of chronic disease that is creating a health crisis both nationally and globally. Because chronic disease is a food- and lifestyle-driven, environment- and genetics-influenced phenomenon, we must have an approach to care that integrates all these elements in the context of the patient’s complete story. Functional Medicine does just that and provides an original and creative approach to the collection and analysis of this broad array of information. Using all the concepts and tools that IFM has developed, Functional Medicine practitioners contribute vital skills for treating and reversing complex, chronic disease.
Sourced From:
The Global Leader in Functional Medicine
References
1 Centers for Disease Control and Prevention. Accessed April 14, 2017, https://www.cdc.gov/chronicdisease.
2 Centers for Medicare & Medicaid Services. NHE Fact Sheet. Accessed April 14, 2017, https://www.cms.gov/research-statistics-data-and-systems/statisticstrends-and-reports/nationalhealthexpenddata/nhe-fact-sheet.html.
3 DeVol R, Bedroussian A. An unhealthy America: the economic burden of chronic disease—charting a new course to save lives and increase productivity and economic growth. Milken Institute; 2007. Accessed April 14, 2017, http://assets1c.milkeninstitute.org/assets/Publication/ResearchReport/PDF/chronic_disease_report.pdf.
4 Bodenheimer T, Chen E, Bennett H. Confronting the growing burden of chronic disease: can the U.S. health care workforce do the job? Health Aff. 2009;28(1):64-74. doi: 10.1377/hlthaff.28.1.64.
5 Bureau of Labor Education, University of Maine. The U.S. Health Care System: Best in the World, Or Just the Most Expensive? 2001. Accessed April 14, 2017, http://www.suddenlysenior.com/pdf_files/U.S.healthcare.pdf.
6 Radley DC, McCarthy D, Hayes SL. Aiming higher: results from the Commonwealth Fund scorecard on state health system performance (2017 ed.). The Commonwealth Fund; 2017. Accessed April 14, 2017, http://www.commonwealthfund.org/interactives/2017/mar/state-scorecard/.
7 Jones DS, Hofmann L, Quinn S. 21st century medicine: a new model for medical education and practice. Gig Harbor, WA: The Institute for Functional Medicine; 2011.
8 Jones DS, Hofmann L, Quinn S. 21st century medicine: a new model for medical education and practice. Gig Harbor, WA: The Institute for Functional Medicine; 2009.
9 Willett WC. Balancing life-style and genomics research for disease prevention. Science. 2002; 296(5568):695-97. doi: 10.1126/science.1071055.
10 Thorpe KE, Florence CS, Howard H, Joski P. The rising prevalence of treated disease: effects on private health insurance spending. Health Aff. 2005;Suppl Web Exclusives: W5-317-W5-325. doi: 10.1377/hlthaff.w5.317.
11 Heaney RP. Long-latency deficiency disease: insights from calcium and vitamin D. Am J Clin Nutr. 2003;78(5):912-9.
12 Lazarou J, Pomeranz BH, Corey PN. Incidence of adverse drug reactions in hospitalized patients: a meta-analysis of prospective studies. JAMA. 1998; 279(15):1200-05.
13 Ames BN, Elson-Schwab I, Silver EA. High-dose vitamin therapy stimulates variant enzymes with decreased coenzyme binding affinity (increased K(m)): relevance to genetic disease and polymorphisms. Am J Clin Nutr. 2002;75(4):616-58.
14 Lands B. Prevent the cause, not just the symptoms. Prostaglandins Other Lipid Mediat. 201;96(1-4):90-3. doi: 10.1016/j.prostaglandins.2011.07.003.
15 Sofi F, Abbate R, Gensini GF, Casini A. Accruing evidence on benefits of adherence to the Mediterranean diet on health: an updated systematic review and meta-analysis. Am J Clin Nutr. 2010;92(5):1189-96. doi: 10.3945/ajcn.2010.29673.
16 Mulrow C, Lawrence V, Jacobs B, et al. Milk thistle: effects on liver disease and cirrhosis and clinical adverse effects (No. 21). Rockville, MD: Agency for Healthcare Research and Quality; 2000. Accessed April 14, 2017, http://www.pkids.org/files/milkthistle.pdf.
17 National Center for Complementary and Integrative Health. Green Tea; 2016. Accessed April 14, 2017, https://nccih.nih.gov/health/greentea.
18 National Center for Complementary and Integrative Health. St. John’s Wort; 2016. Accessed April 14, 2017, https://nccih.nih.gov/health/stjohnswort/ataglance.htm.
19 McArdle WD, Katch EI, Katch VL. Exercise Physiology: Energy, Nutrition, and Human Performance. Philadelphia: Lippincott Williams and Wilkins; 2001.
20 McCraty R, Childre D. Coherence: bridging personal, social, and global health. Altern Ther Health Med. 2010;16(4):10-24.
21 Yi B, Kasai H, Lee HS, Kang Y, Park JY, Yang M. Inhibition by wheat sprout (Triticum aestivum) juice of bisphenol A-induced oxidative stress in young women. Mutat Res. 2011;724(1-2):64-68. doi: 10.1016/j.mrgentox.2011.06.007.
22 Johnson CH, Patterson AD, Idle JR, Gonzalez FJ. Xenobiotic metabolomics: major impact on the metabolome. Annu Rev Pharmacol Toxicol. 2012;52:37-56. doi: 10.1146/annurev-pharmtox-010611-134748.
23 Scapagnini G, Caruso C, Calabrese V. Therapeutic potential of dietary polyphenols against brain ageing and neurodegenerative disorders. Adv Exp Med Biol. 2010;698:27-35.
24 Colak MC, Kavakli A, Kilinç A, Rahman A. Postoperative pain and respiratory function in patients treated with electroacupuncture following coronary surgery. Neurosciences (Riyadh). 2010;15(1):7-10.
25 Cao H, Pan X, Li H, Liu J. Acupuncture for treatment of insomnia: a systematic review of randomized controlled trials. J Altern Complement Med. 2009;15(11):1171-86. doi: 10.1089/acm.2009.0041.
26 Lee A, Fan LT. Stimulation of the wrist acupuncture point P6 for preventing postoperative nausea and vomiting. Cochrane Database Syst Rev. 2009;15(2):CD003281. doi: 10.1002/14651858.
27 Rubinstein SM, Leboeuf-Yde C, Knol DL, de Koekkoek TE, Pfeifle CE, van Tulder MW. The benefits outweigh the risks for patient undergoing chiropractic care for neck pain: a prospective, multicenter, cohort study. J Manipulative Physiol Ter. 2007;30(6):408-1. doi: 10.1016/j.jmpt.2007.04.013.
28 Beyerman KL, Palmerino MB, Zohn LE, Kane GM, Foster KA. Efficacy of treating low back pain and dysfunction secondary to osteoarthritis: chiropractic care compared to moist heat alone. J Manipulative Physiol Ther. 2006;29(2):107-14. doi: 10.1016/j.jmpt.2005.10.005.
29 Kshettry VR, Carole LF, Henly SJ, Sendelbach S, Kummer B. Complementary alternative medical therapies for heart surgery patients: feasibility, safety, and impact. Ann Thorac Surg. 2006;81(1):201-5. doi: 10.1016/j.athoracsur.2005.06.016.
30 Ornish D, Magbanua MJM, Weidner G, et al. Changes in prostate gene expression in men undergoing an intensive nutrition and lifestyle intervention. PNAS. 2008;105(24):8369-74. doi: 10.1073/pnas.0803080105.
31 Xiong GL, Doraiswamy PM. Does meditation enhance cognition and brain plasticity? Ann NY Acad Sci. 2009;1172:63-9. doi: 10.1196/annals.1393.002.
32 Hölzel BK, Carmody J, Vangel M, et al. Mindfulness practice leads to increases in regional brain gray matter density. Psychiatry Res. 2011;191(1):36-43. doi: 10.1016/j.pscychresns.2010.08.006.
Post Disclaimer
Professional Scope of Practice *
The information herein on "What Is Functional Medicine: An Introduction" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness, Personal Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those on this site and our family practice-based chiromed.com site, and focuses on restoring health naturally for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
Licenses and Board Certifications:
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card



 Constructing The Model & Putting It Into Practice
Constructing The Model & Putting It Into Practice

 Again, We Welcome You.
Again, We Welcome You.
Comments are closed.