Table of Contents
Ankle Fractures
- 10% of all fractures. 2nd m/c following femoral neck Fx. Demographics: young active males and older osteoporotic females
- Stable Fx: overall prognosis is good
- Unstable Fx: require ORIF. 15%-20% chances of 2nd OA.
- Role of imaging is to determine the complexity, stability and care planning (i.e. operative vs. conservative)
- Weber classification considers tearing of distal tibial-fibular syndesmosis and potential instability
- Weber A – below syndesmosis. Stable, typically avulsion of distal fibular malleolus
- Weber B – at the level of syndesmosis: may be outside syndesmosis and stable or tearing syndesmosis and unstable
- Weber C – above syndesmosis. Always nstable d/t tearing of syndesmosis
- Variations of fractures may involve the postition/role of the talus bone during Fx (e.g. abduction, adduction, rotation etc.) this is known as Lauge-Hanson classification
Tibiofibular Syndesmosis & Ankle Stability
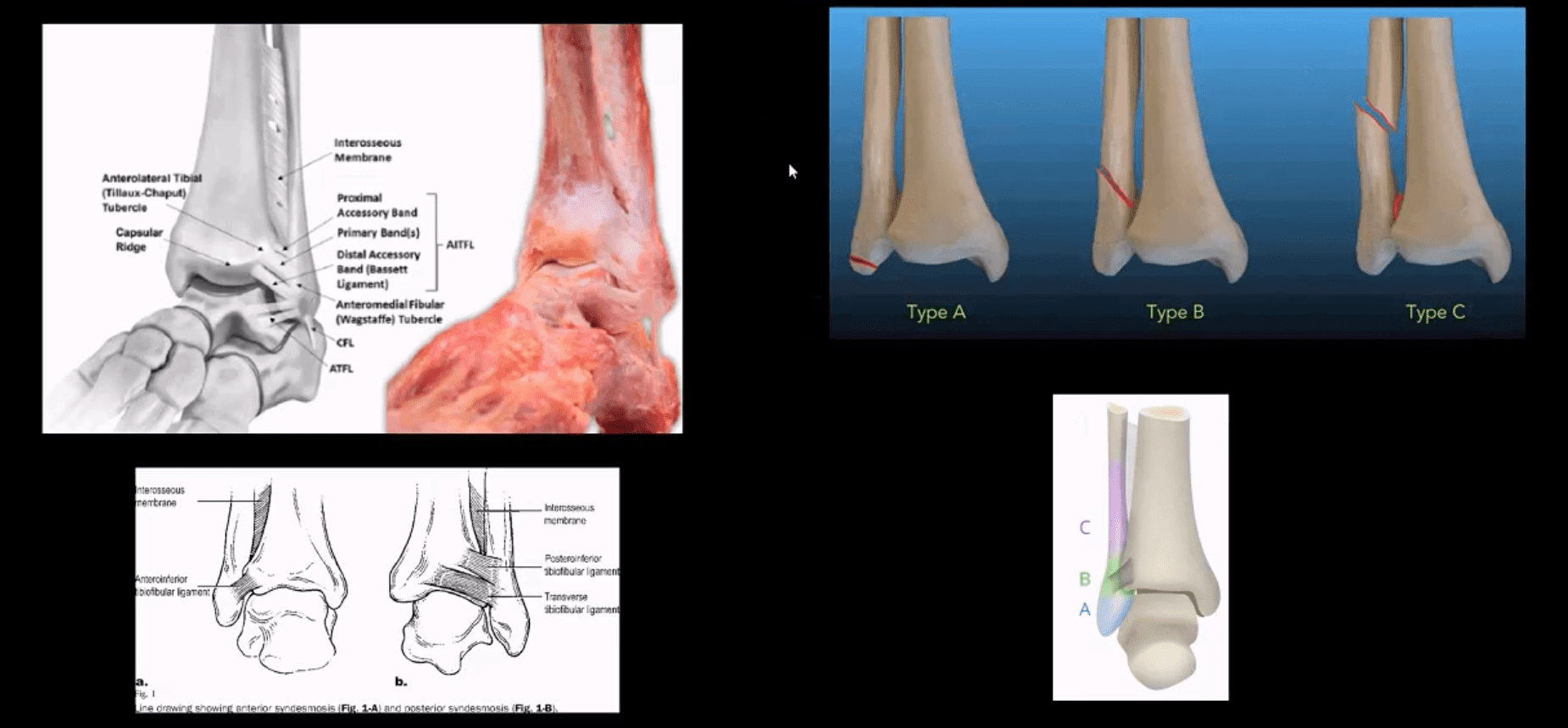
- Denis-Weber classification of ankle fractures
Clinical Dx Accuracy
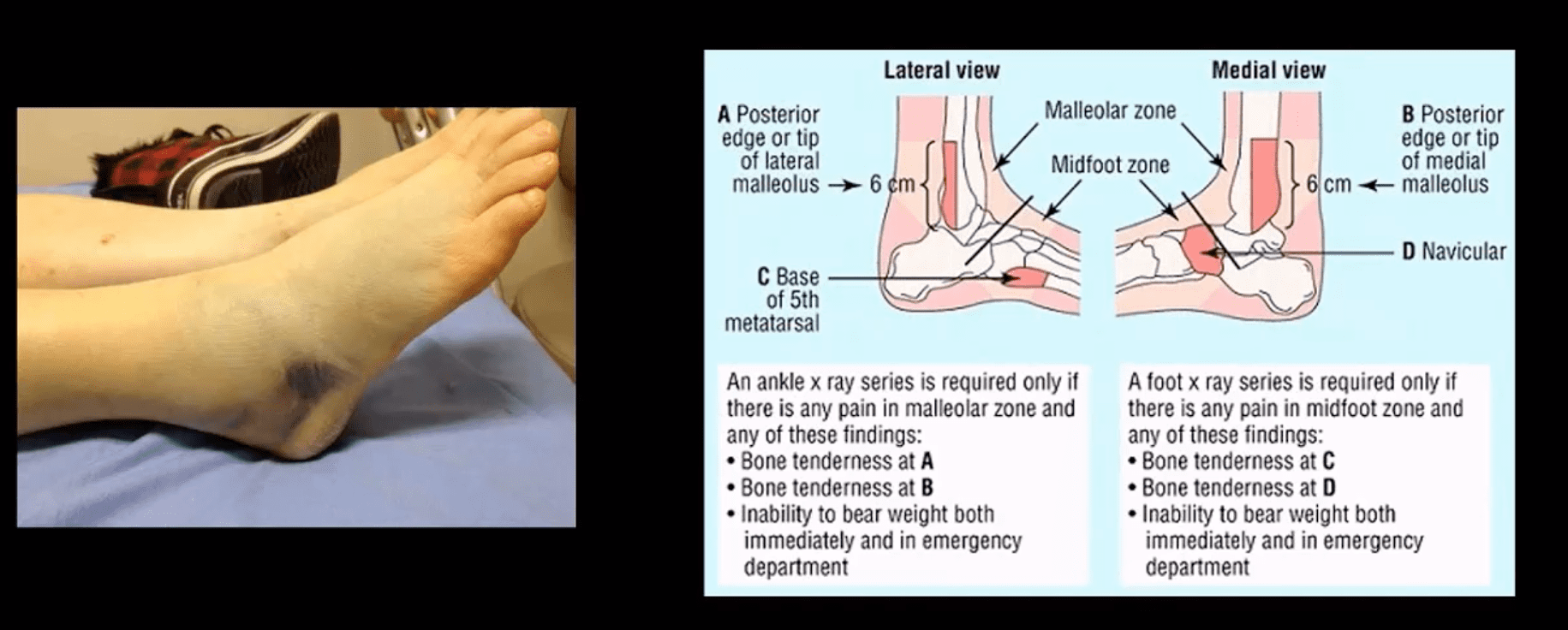
- Ankle Fractures could be facilitated by the “Ottawa Rule“
Mortise & AP Views
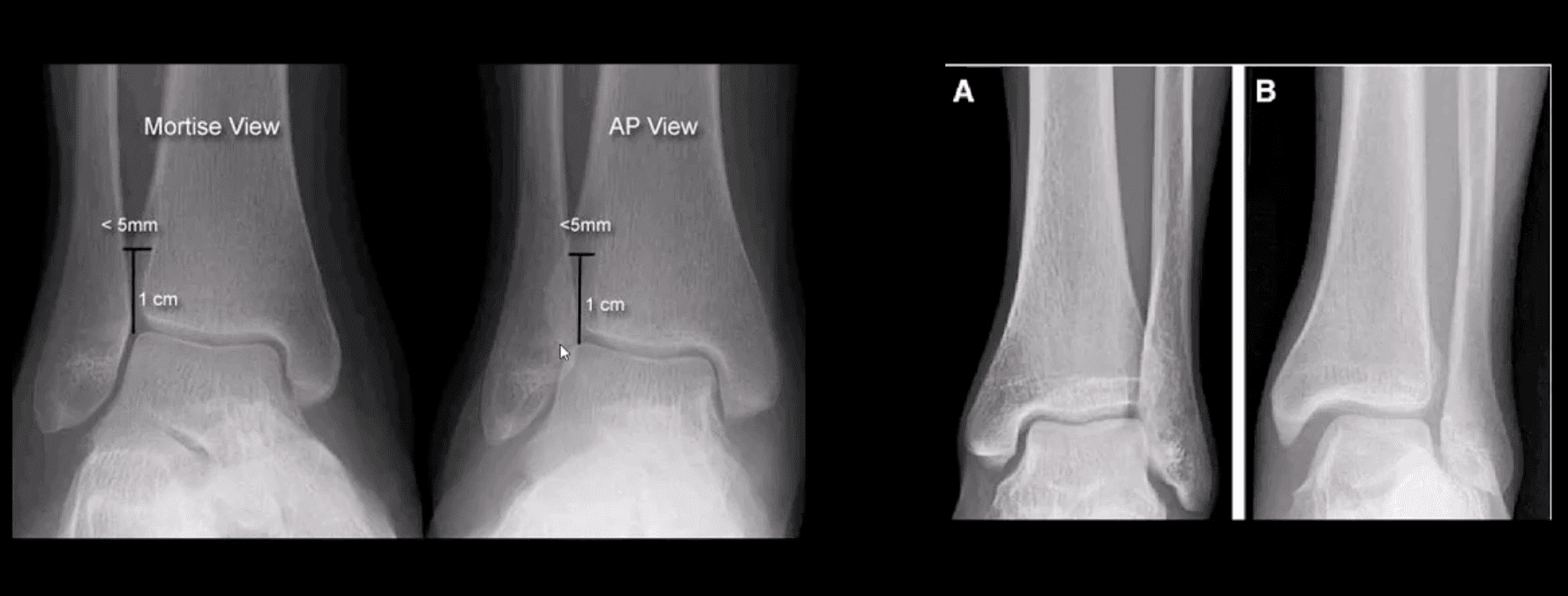
AP, Medial Oblique & Lateral Views
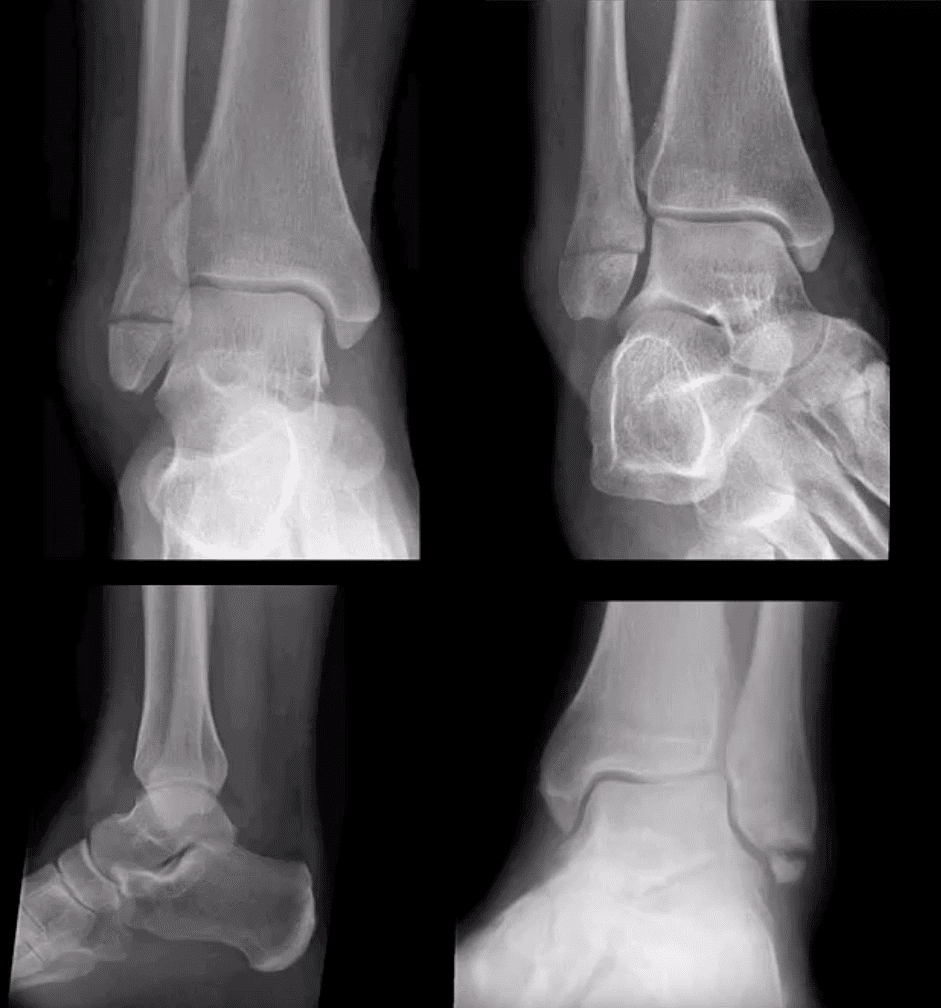
- Reveal infrasyndesmotic Fx of fibular malleolus (Weber A)
- Stable Injury
- Conservative care in the form of short-leg walking cast/boot can be used. Good recovery. If no evidence of ostechondral injury, relatively low chances of post-traumatic OA
- No further imaging required. MRI may help to reveal bone contusion and osteochondral injury
Weber B at Level of Syndesmosis
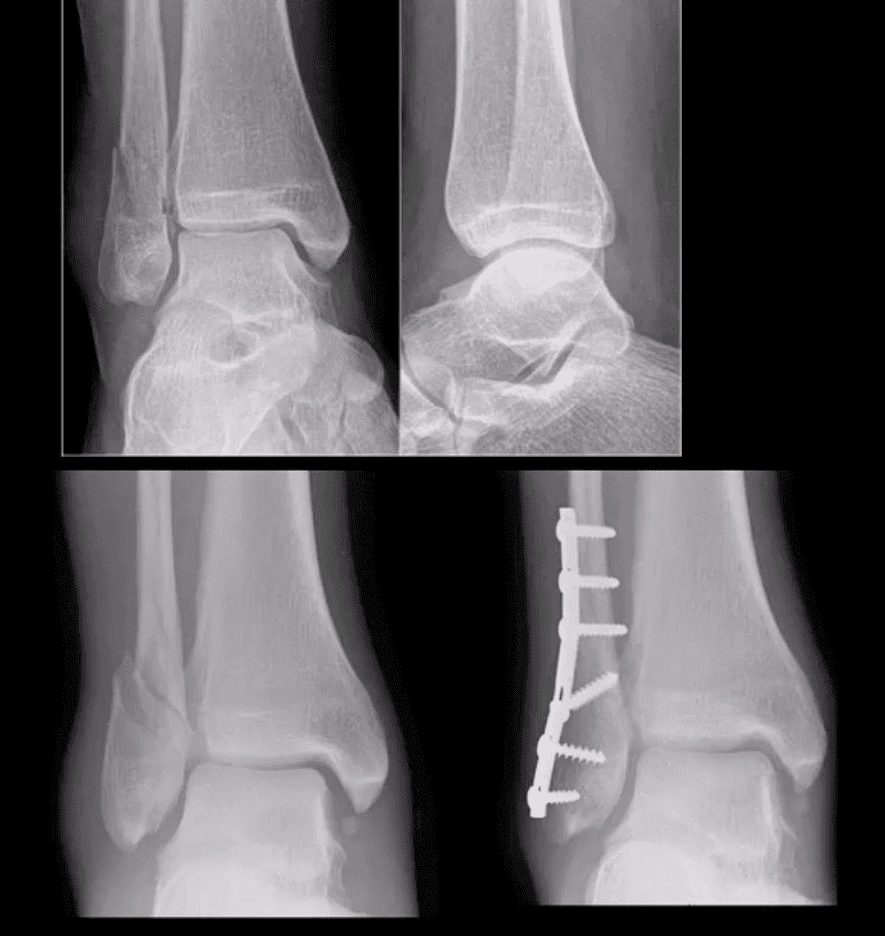
- Can be stable or unstable. On occasions, the decision is made during operative exploration.
- CT scanning may help with further evaluation
- Management: depends on stability. Additional stabilization required if syndesmosis is ruptured
Weber C
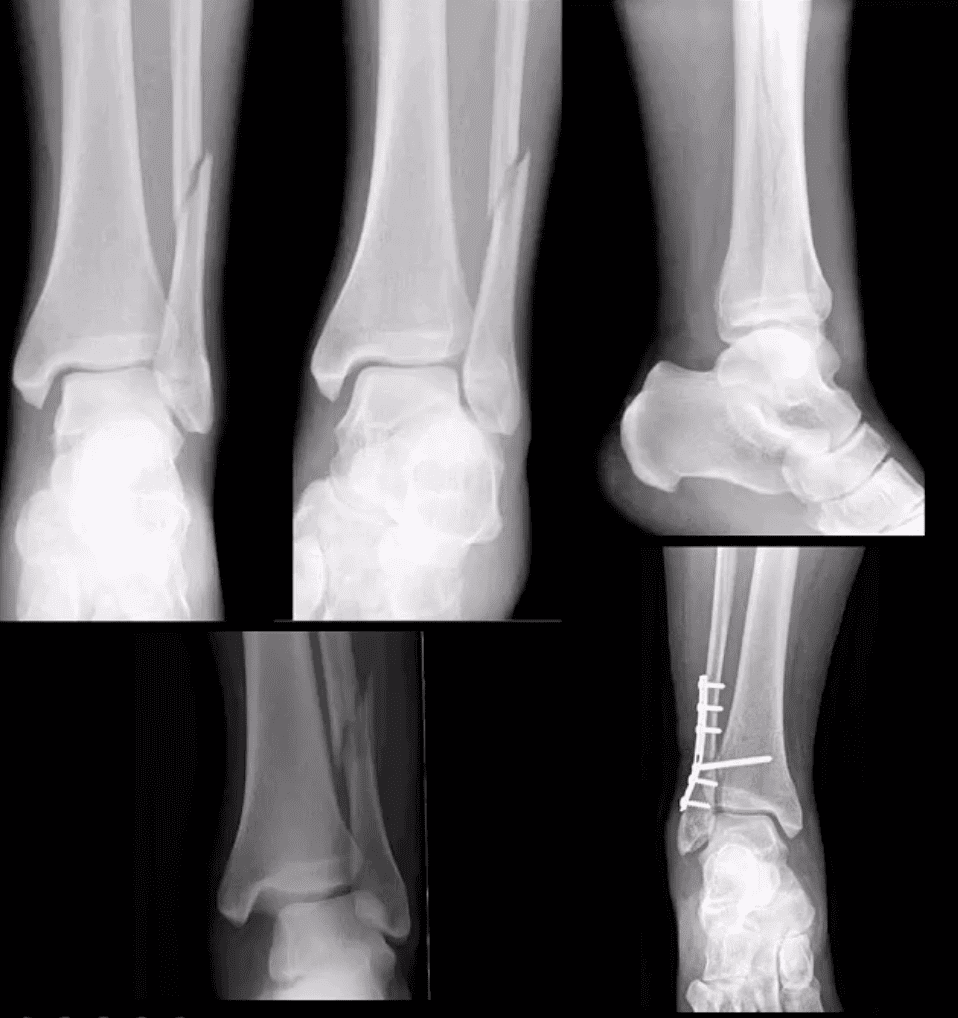
- AP, medial oblique and lateral views reveal Weber C – suprasyndesmotic injury with abnormal joint widening d/t disruption of tib-fib syndesmosis. Very unstable injury.
- Occasionally, when Weber C Fx positioned 6-cm from the tip of the lateral malleolus it may be termed as Pott’s ankle Fx (name after Percival Pott’s who has porposed the original classification of ankle fractures based on their stability and degree of rotation). The term is somewhat outdated.
- Management: operative with additional stabilization of the syndesmosis
Maisonneuve Fracture
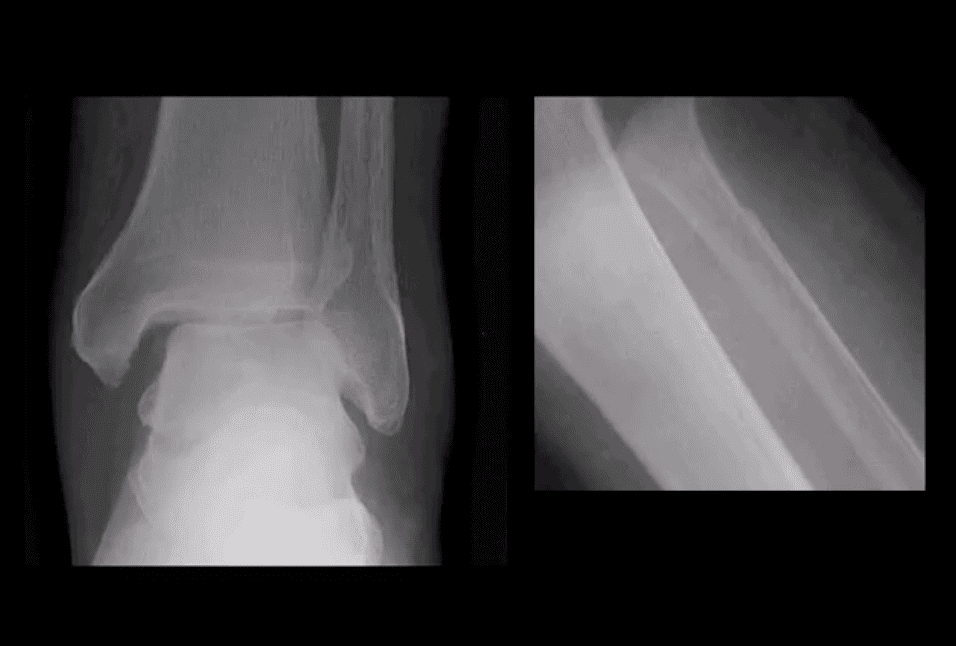
- Often spiral fracture of the proximal fibula combined with an unstable ankle injury
- No immediate ankle fracture is noted radiographically, thus can be missed on ankle views and require tibia and fibula views
- Rad features: widening of the ankle d/t syndesmosis tear and sometimes deltoid ligament disruption. Interosseous membrane is torn with proximal fibular Fx caused by pronation with external-rotation force
- Management: operative
Bimalleolar & Trimalleolar Fx
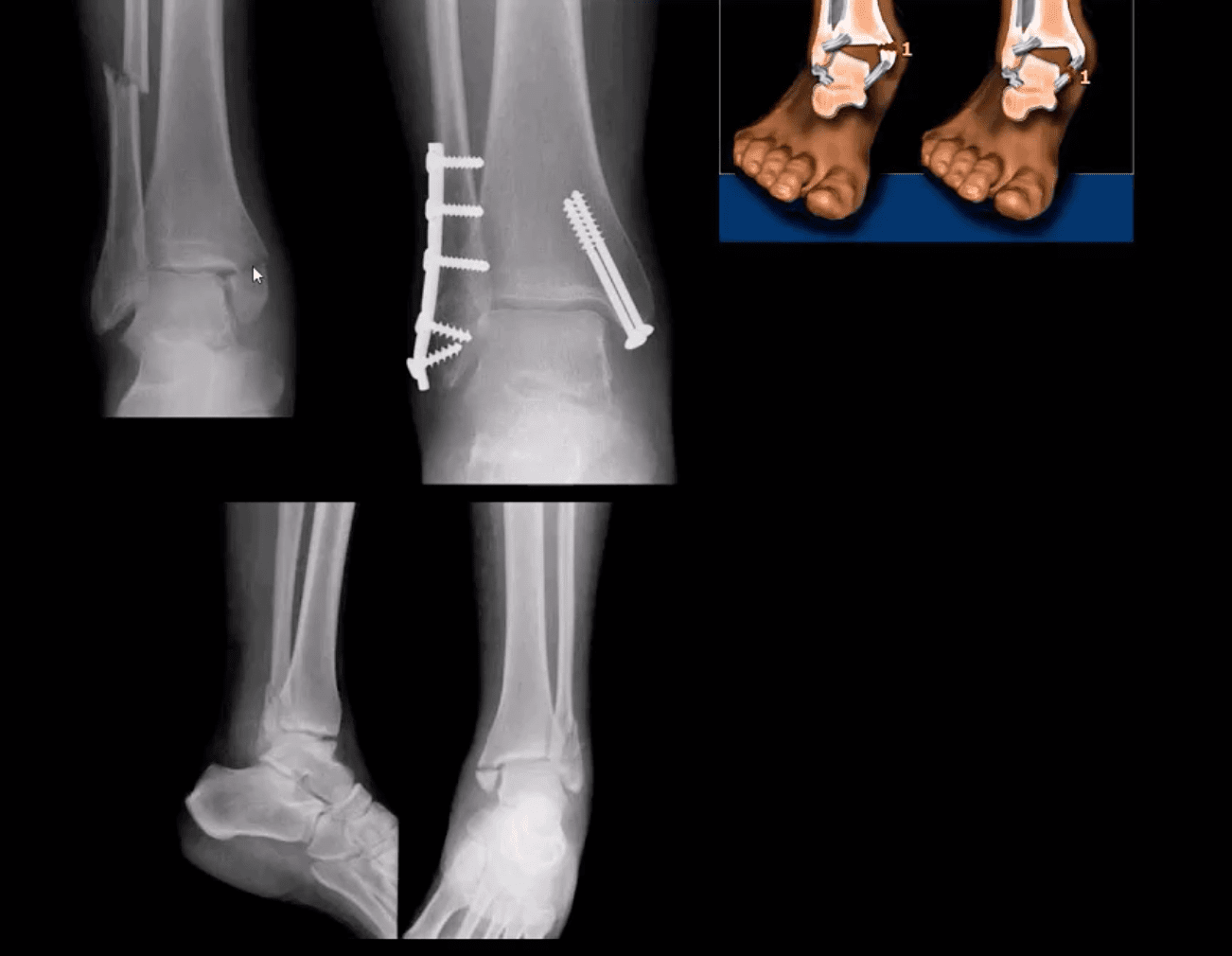
- Above top images Bimalleolar Fx v. unstable, result of pronation and abduction/external rotation. Rx: ORIF.
- Trimalleolar Fx: 3-parts ankle Fx. Medial and lateral malleolus and avulsion of theposterior aspect of tibial plafond. More unstable. Rx: operative
Tillaux Fx
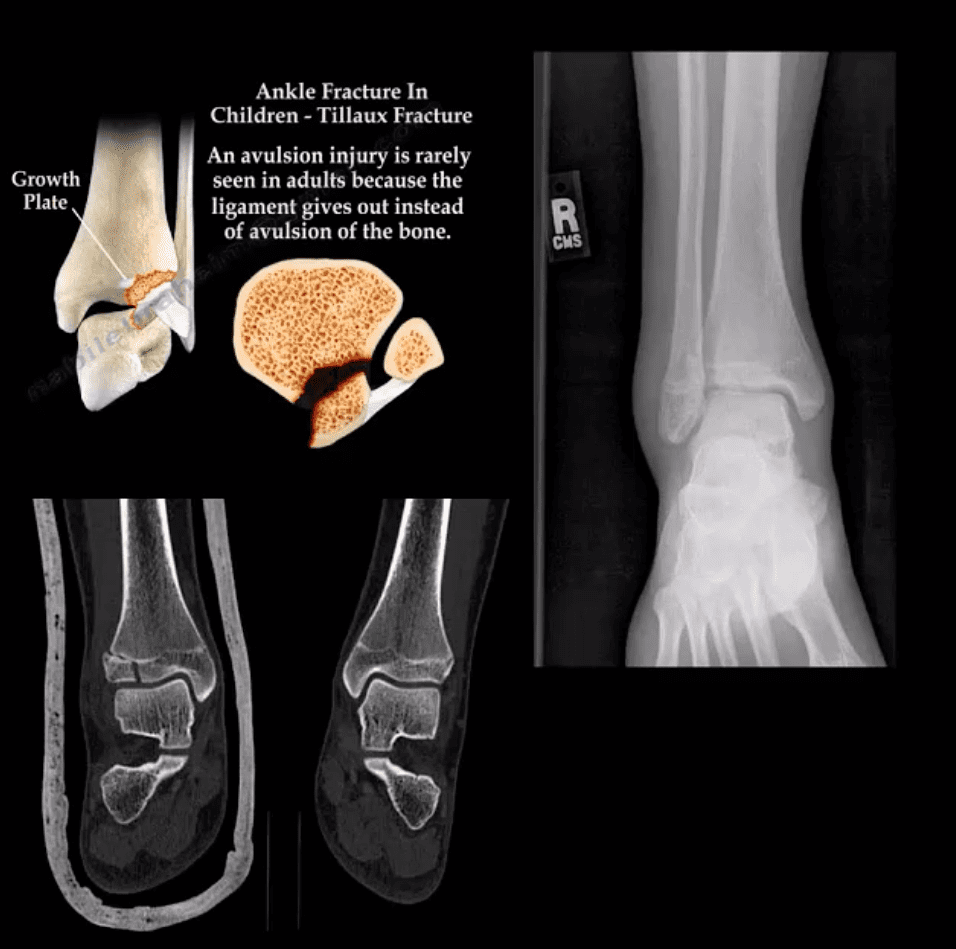
- Pediatric Fx affecting older child when medial side of the physis is closed or about to close with lateral side till open. Avulsion by anterior tibi-fibular ligament. Complications: 2nd dry/premature OA. Rx: can be conservative if stable by boot cast immobilization.
Pediatric Growth Plate Injuries
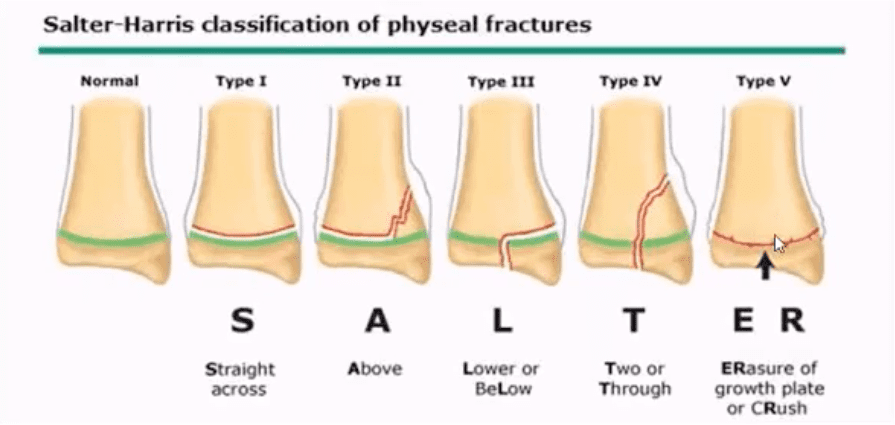
- Salter-Harris classification helps to diagnose and prognosticate physeal injuries.
- Helpful mnemonic: SALTR
- S: type 1-slip through growth plate
- A: type 2-above, Fx extends into metaphysis
- L: type 3-lower, intra-articular Fx extends through the epiphysis
- T: type4, “through” Fx extends through all: physis, metapysis and epiphysis.
- R: type 5, “ruined.” Crush injury to physis leading to complete death of teh growth plate
- Type 1 and 5: present with no fracture
- Type 2: has the best prognosis and considered the most common.
- Management: referral to pediatric orthopedic surgeon
- Complications: early physis closure, limb shortening, premature OA and others.
Calcaneal Fracture
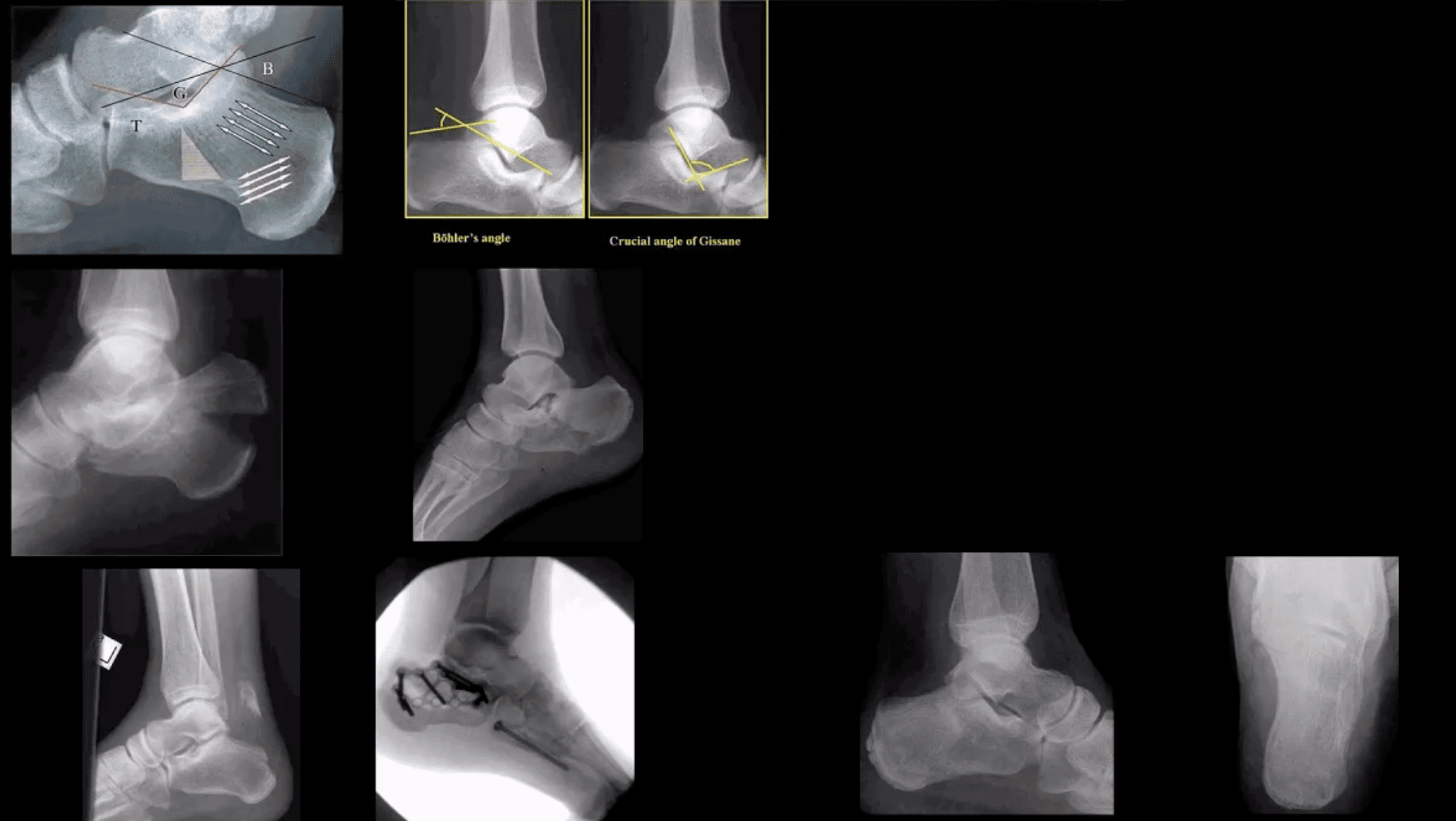
- Most frequent tarsal Fx. 17% open Fx
- Mechanisms: axial loading (intra-articular Fx into sub-talar and calcaneal-cuboid joints in 75% cases). Avulsion by Achilles tendon (m/c in osteoporotic bone). Stress (fatigue) Fx.
- Intra-articular Fx carries a poor prognosis. Typically comminuted. Rx: operative.
- B/I calcaneal intra-articular fx with associated vertebra compression Fx with associated vertebral compression Fx (T10-L2) often termed Casanova aka Don Juan (Lover’s) fx.
- Imaging: x-radiography with added “heel view” 1st step. CT scanning is best for Dx and pre-op planning.
- Radiography: Bohler’s angle (<20-degrees) Gissane angle >130-degrees. Indicate Calcan, Fx.
Tarsal Bones
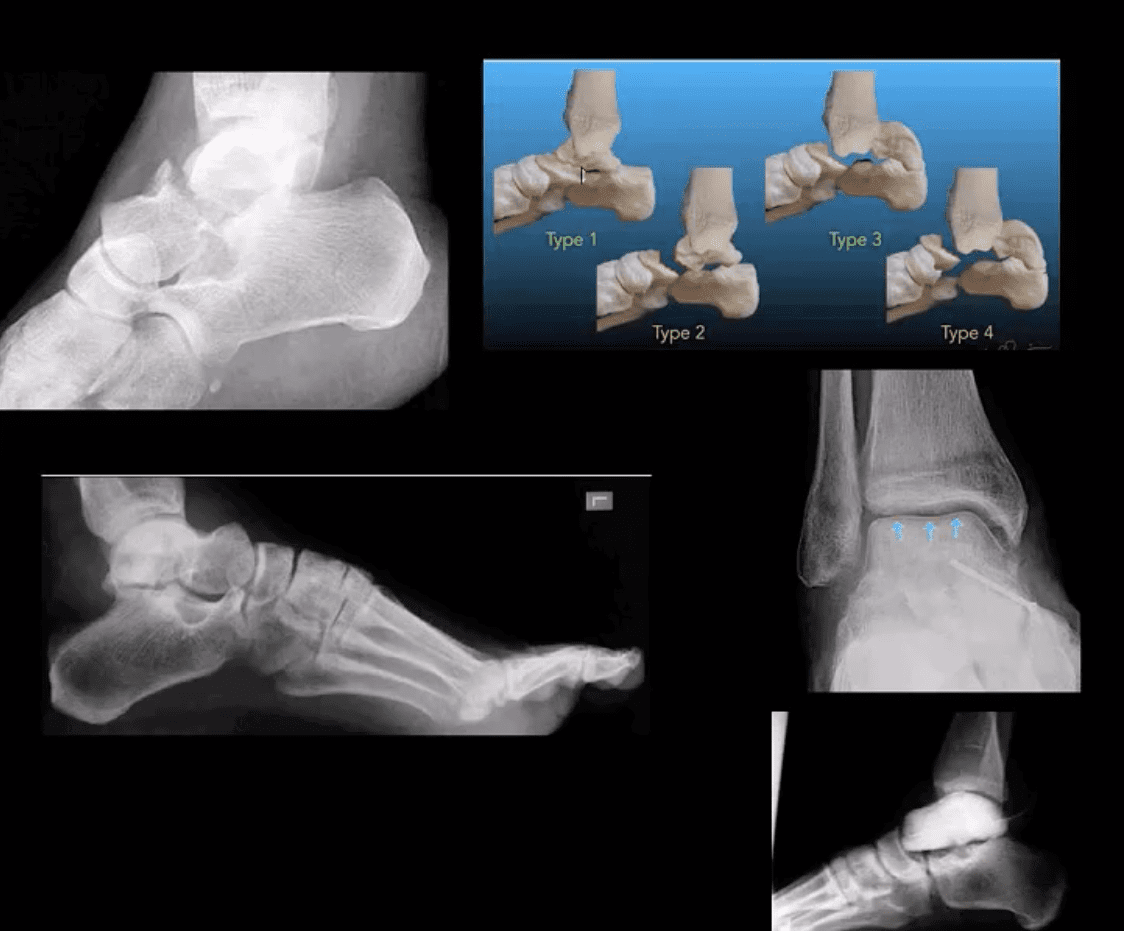
- M/C fractured tarsal bone is the Talus. M/C region: talar neck (30-50%). Mechanism: Axial loading in dorsiflexion. Complications: Ischemic osteonecrosis (AVN) of the talus. Premature (2nd OA). Imaging: 1st step: radiographs, CT can be helpful with further delineation
- Hawkins classification helps with Dx, prognosis & treatment. “Hawkins sign’ on plain film/CT scan may help with AVN Dx. (above blue arrows indicate good prognosis d/t radioluncent line indicating no AVN because bone is vascularized and hence resorbed)
- Rx: Type 1: conservative with short leg cast or boot (risk of AVN-0-15%), Type 2-4-ORIF (risk of AVN 50%-100%)
Ankle & Foot Imaging
Post Disclaimer
Professional Scope of Practice *
The information herein on "Ankle & Foot Diagnostic Imaging Arthritis & Trauma I | El Paso, TX." is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness, Personal Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those on this site and our family practice-based chiromed.com site, and focuses on restoring health naturally for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
Licenses and Board Certifications:
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card




 Again, We Welcome You.
Again, We Welcome You.
Comments are closed.